Campylobacter was the top cause of illness while E. coli numbers reached a record high last year, according to foodborne illness figures from Switzerland.
The 2018 surveillance report of zoonoses and outbreaks of food poisoning revealed a decline in Salmonella and a slight increase in Listeria with only a dozen foodborne outbreaks reported.
In 2018, campylobacteriosis remained the most frequently recorded zoonosis in humans. A total of 7,675 cases confirmed by laboratory diagnosis were reported. This represents a slight increase over 7,219 cases in the previous year. People usually become infected by eating contaminated food, with poultry meat being the primary source of infection.
As in previous years, young adults (aged 15-24) had the highest reporting rate and the rate for over-64s was also high. Men were slightly more affected than women.
The peak was reached in July and August, with 2,056 cases. This is due to the summer grilling season and more trips abroad. Like past years, a second short-term increase during the Christmas and New Year holidays was attributed to consumption of the Swiss version of Chinese fondue.
Campylobacter jejuni made up 69 percent of the 5,688 cases were species information was available while Campylobacter coli was responsible for 9 percent.
In self-monitoring by the poultry sector, 1,776 analyzes were done on chicken and turkey meat in 2018. Of these, 436 (24.5 percent) were positive for Campylobacter spp. compared to 27 percent in 2017.
Salmonella on the slide
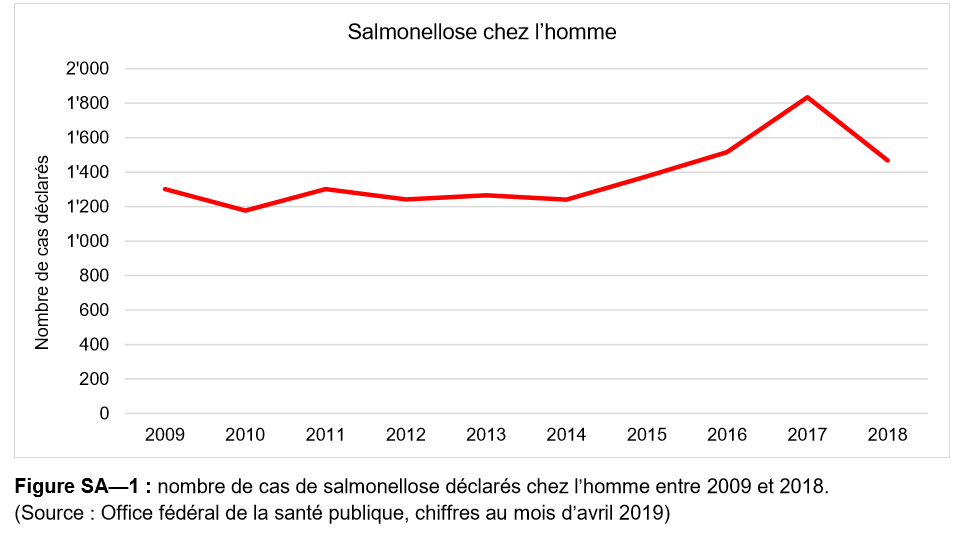
In 2018, 1,467 laboratory-confirmed cases of salmonellosis were reported which was a decrease compared to 1,835 cases in the previous year.
As in previous years, most infections were in children aged less than 5 years old. Seasonal peaks in summer and autumn months occurred again in 2018. The most frequently reported serovars were the same: Enteritidis, followed by S. Typhimurium and the monophasic strain 4.12: 1: -.
As part of self-monitoring by the poultry sector, 3,712 analyzes were conducted on chicken and turkey meat including carcasses and meat samples. In total, 12 of them were positive for Salmonella. There were five cases of Albany, four of Typhimurium and one each of Enterica, Chester, and Infantis.
Cases of salmonellosis declined from more than 6,000 per year in the early 1990s to about 1,300 annual infections in 2009. From 2009 to 2014, the number was stable but for an unknown reason, it has been on the rise since 2015.
E. coli at a record high
With 822 confirmed cases, the year was marked by a further increase in verotoxigenic E. coli (VTEC) or Shiga toxin-producing E. coli (STEC) infections in humans versus the 696 reports in 2017. Infection rate is the highest since the introduction of reporting obligation in 1999. The main cause of this increase is likely to be laboratories are testing more and can detect more cases because of new methods of analysis.
As in 2017, most cases were in the third quarter. Children under the age of 5 still have the highest reporting rates although the
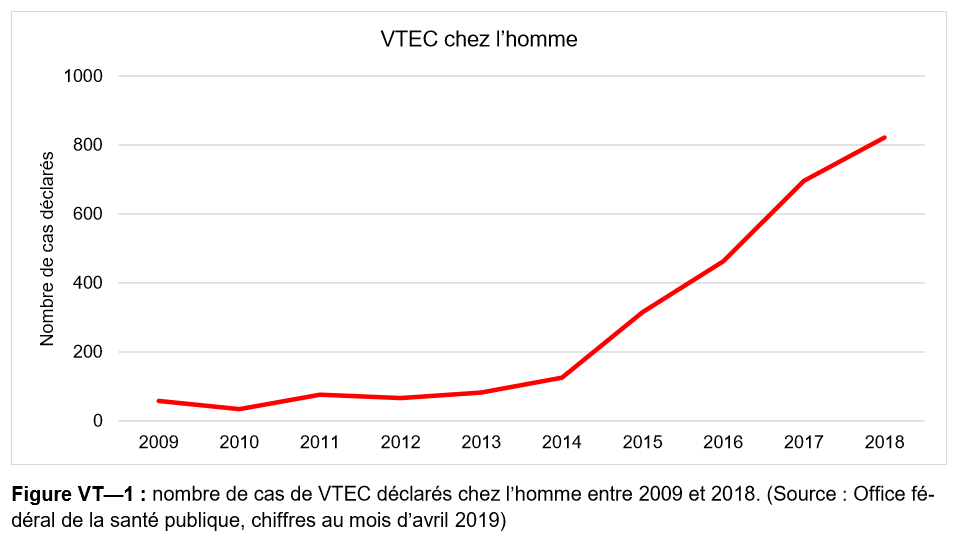
rate in people aged 65 and over has risen sharply in recent years. In all age groups, women were slightly more affected than men.
The most frequently detected serogroups, for the 219 cases with available data, are O157 (17 cases), O146 (15), O103 (14), O91 (13) and O26 (10). Last year, 23 cases of the hemolytic uremic syndrome (HUS) were reported which was up from 19 in 2017. Children under 5 years old and adults aged 64 and over were particularly affected.
In 2017, VTEC was detected in 2 percent of 51 raw milk kinds of cheese analyzed and 1.9 percent of 53 raw meat products tested. None of 73 samples of raw milk sold directly on the farm revealed E. coli.
In 2018, the presence of VTEC was analyzed in 70 flour samples. Nine were positive for the verotoxin gene (VTX). Eight isolated VTEC strains belonged to six different serotypes including O103: H2, O146: H28 or O11: H48) and different subtypes of VTX were identified.
Listeria at a level
Last year, 52 listeriosis cases confirmed by laboratory diagnosis were reported, which was a slight rise from the year before. One case of transmission from mother to child was reported.
As in previous years, the highest reporting rate was in the over-64 age group. The serotype was known for 51 cases. The most common was 1/2a and 4b with 24 cases of each.
Twelve cases of listeriosis serotype 4b were also recorded with a close relationship based on genome sequencing. This outbreak was likely caused by a foodstuff of common origin but an investigation did not find the source.
In 2018, 1,342 cheese, 171 environmental and 26 milk samples were tested for Listeria. Listeria monocytogenes was detected in two samples from the surface of a cheese. Other strains were found in 16 samples.
A total of 1,000 samples of ready-to-eat foods were also sampled from the Swiss market and Listeria monocytogenes was present in 3 percent of them but not at levels above legal limits.
Five cases of brucellosis confirmed by laboratory diagnosis were reported compared to nine in 2017. These cases involved two men and three women aged 38 to 72 years. In two, the agent was identified as Brucella melitensis.
Infections are often related to trips abroad or consumption of foreign dairy products. The Swiss dairy cattle herd is free from brucellosis. However, raw milk must be heated to at least 70 degrees Celsius before consumption.
A low number of outbreaks
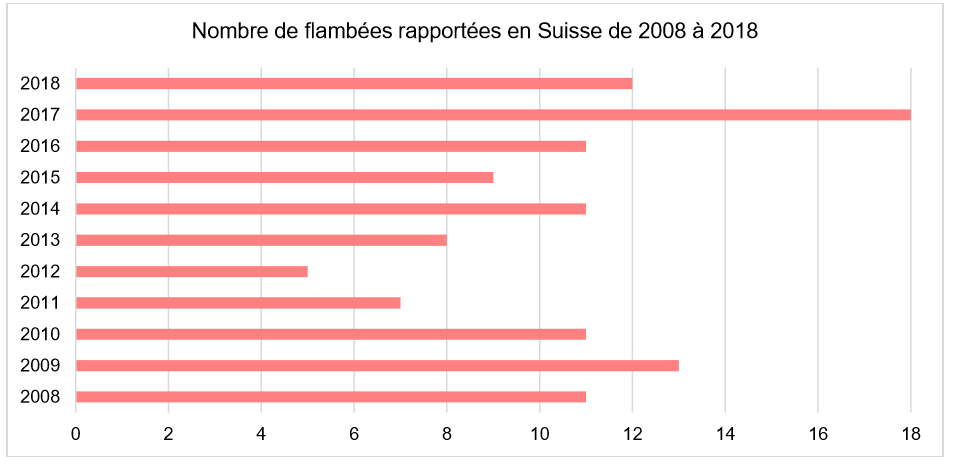
Foodborne outbreaks have been rare in Switzerland for several years. Only 12 were reported for 2018 compared to 18 the previous year. In these dozen incidents, more than 153 people became ill and at least five were hospitalized. In seven cases it was not possible to identify the infectious agent. In the largest outbreak, 73 soldiers belonging to a military school fell ill in one night with gastrointestinal pain and sometimes diarrhea and vomiting but an investigation did not identify the agent or source.
Chili oil with a pulled pork sandwich caused an outbreak of Salmonella Weltevreden at a Street Food Festival. Three of the four patients had severe and long-lasting symptoms and needed to be hospitalized. Seven people were sick from Salmonella enteritidis at a private house after having an omelet and eight fell ill after eating at a restaurant where Salmonella from a chocolate mousse made with raw eggs was suspected.
In one of the other outbreaks, Bacillus cereus at more than 49,000 colony forming units per gram (CFU/g) was detected in rice served in a restaurant that sickened four people.
Finally, after a meal served by a caterer, 10 out of 16 people became ill. All had consumed the same soup which was later found to contain Staphylococcus aureus at 1,700 CFU/g. Other bacteria – such as Bacillus cereus and Enterobacteriaceae – were found in dishes accompanying the soup but were excluded as the source of illness because they were not eaten by all patients.
(To sign up for a free subscription to Food Safety News, click here.)









