Campylobacter, Yersinia, E. coli and Listeria infections all went up while Salmonella declined, according to the 2018 report on foodborne disease in New Zealand.
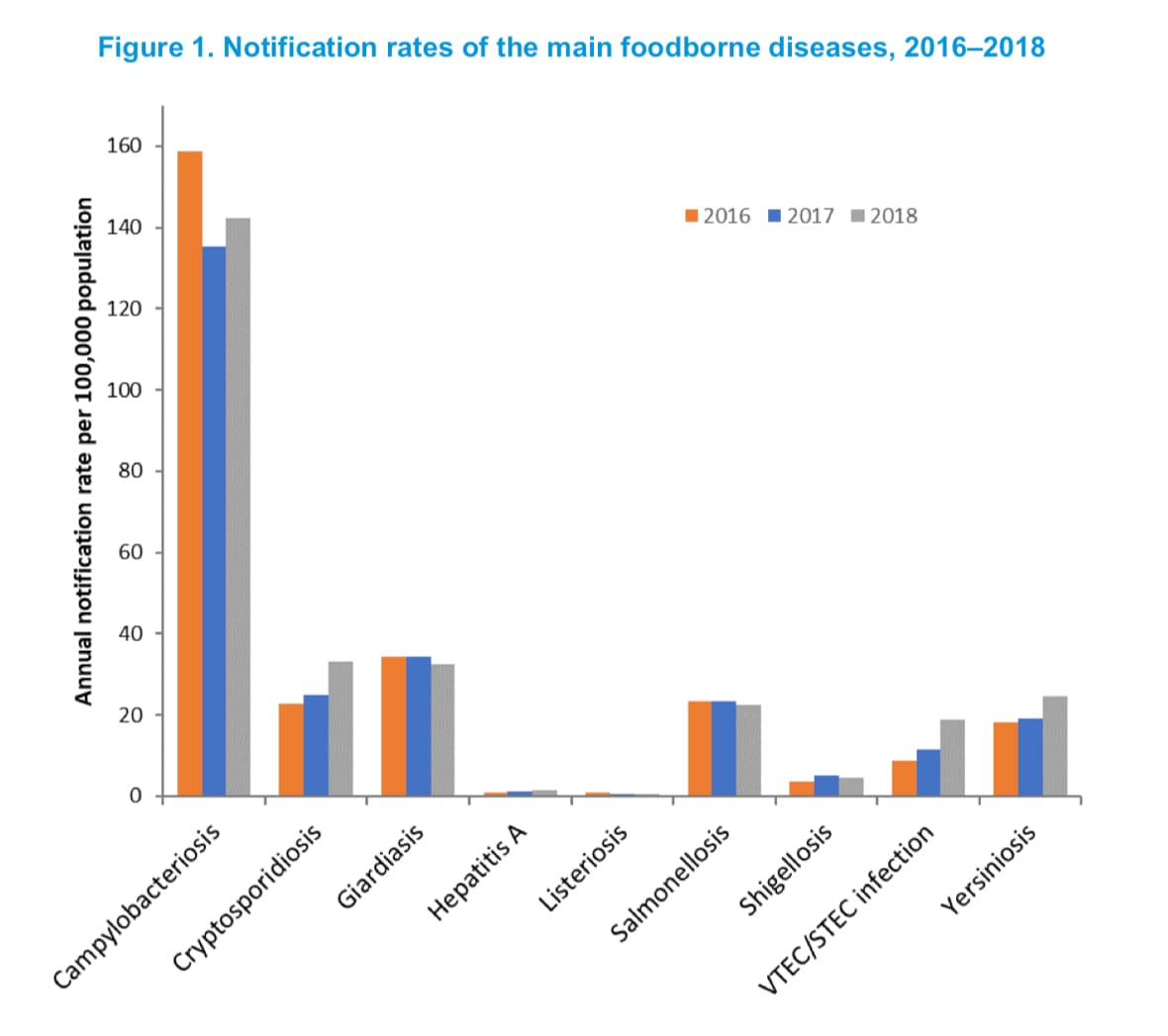
Campylobacter remained the top foodborne pathogen. The country has a performance target to reduce cases of foodborne campylobacteriosis by 10 percent from 88.4 to 79.6 per 100,000 per head of population by the end of 2020. The estimated incidence in 2018 was 78.3 per 100,000.
New Zealand Food Safety (NZFS) is part of the Ministry for Primary Industries (MPI) and leads the country’s food safety system. EpiSurv is the country’s notifiable disease surveillance system.
The shift to culture-independent diagnostic tests (CIDT) using molecular polymerase chain reaction (PCR) methodology for detecting pathogens by medical laboratories in New Zealand continued in 2018.
Shiga toxin-producing E. coli (STEC) infection, shigellosis and cryptosporidiosis notification rates continued to rise sharply as more labs implement CIDT, despite no evidence foodborne sources are increasing.
Rates for campylobacteriosis and salmonellosis remain constant, which may reflect a balance between a possible increase in detection sensitivity using CIDT and reduction in foodborne illness as NZFS and industry implement pathogen control measures, according to the report.
Forty-three foodborne outbreaks with 580 infections occurred in 2018 with the pathogen not identified in 14 instances. Eight were caused by norovirus, seven by Campylobacter, five by Salmonella, three by Hepatitis A, two by histamine and one each by Clostridium perfringens, Shigella, Staphylococcus aureus and Yersinia.
Raw milk link in Campylobacter outbreaks
During 2018, 6,957 cases of campylobacteriosis and no deaths were reported in EpiSurv but 780 people needed hospital treatment. A total of 6,482 Campylobacter infections were recorded in 2017.
It has been estimated by expert consultation that 63.8 percent of campylobacteriosis incidence is due to foodborne transmission, meaning 3,826 infections last year, and 75.4 percent of these are due to poultry.
The number of notifications ranged from 395 in April to 918 in December. The highest age-specific notification rates were for children aged 1 to 4 years and infants less than 1 year. The top hospitalization rates were for the 70 and over age group and infants aged less than 1 year.
Seven of 16 outbreaks caused by Campylobacter spp. and 24 of 92 associated cases were reported as foodborne. Raw milk was confirmed as the vehicle of infection in one outbreak and suspected in three others while duck rillette was implicated in the other outbreak.
During 2009 to 2018, except 2014, the number of foodborne outbreaks has ranged between four and 16 each year with between 19 and 77 outbreak-associated cases.
Salmonella’s slight decline
During 2018, 1,100 cases of salmonellosis and no deaths were reported in EpiSurv but 227 people needed hospital treatment. A total of 1,127 Salmonella infections were recorded in 2017.
It has been estimated by experts that 417 salmonellosis infections were due to foodborne transmission with 19 percent of these due to poultry.
The number of notifications ranged from 63 in July to 139 in August. The rate of notifications were higher for males than females but hospitalization rates were similar for both genders. Notification and hospitalization rates were highest for infants aged less than 1 year.
Five of 14 Salmonella outbreaks with 17 cases were classed as foodborne. Salmonella Bovismorbificans was linked to an outbreak caused by undercooked supermarket chicken prepared at home and Salmonella Weltevreden to one involving raw sea cucumber from Samoa. A Salmonella Typhimurium phage type 195 outbreak may have been caused by supermarket roast leg ham.
The number of foodborne outbreaks between 2009 and 2018 ranged from three in 2015 to 12 in 2016 and associated cases varied between 15 in 2017 and 104 in 2012.
Salmonella Typhimurium and Enteritidis were the most common serotypes. Other common serotypes were Bovismorbificans, Brandenburg, Saintpaul and Stanley with an annual rise for Bovismorbificans since 2015.
Large STEC increase but no foodborne outbreaks
During 2018, 925 cases of STEC infection, 41 hospitalizations and two deaths were reported in EpiSurv compared to 547 cases in 2017.
It has been estimated by experts that 29.9 percent of O157 STEC incidence and 34 percent of non-O157 incidence is due to foodborne transmission. The expert consultation also estimated 30 percent of this was due to red meat.
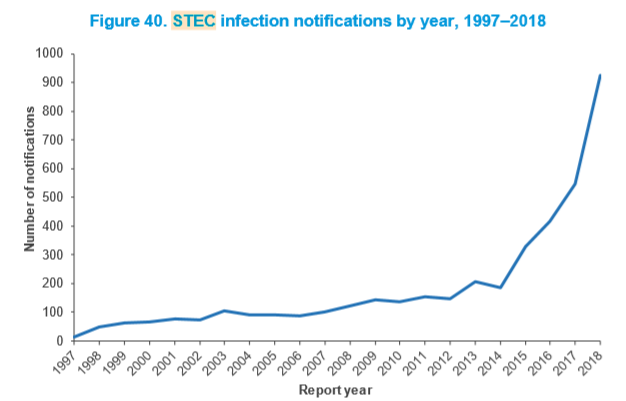
There was a large increase in STEC notifications compared to previous years continuing a trend from 2015. The notification rate in 2018 was about twice as high as the previous three-year average. None of 15 outbreaks with 57 cases were classed as foodborne.
The number of notifications ranged from 42 in June to 122 in February. Notification rates were slightly higher for females than males but hospitalizations were slightly higher for males.
STEC infection notification rate was highest for the less than 1 year age group and the 1 to 4 years age group. The number of hospitalizations was most in the 70+ age group and ranged between zero and six in all other age groups.
The number of foodborne STEC outbreaks between 2009 and 2018 ranged from one to four, with no outbreaks for five of the 10 years. Cases associated with outbreaks has varied over the same period with peaks in 2014 at 15 and 2017 with 157 cases.
A total of 632 cases infected with STEC were reported. Of these, 194 isolates were E. coli O157:H7, 376 non-O157 and for 62 isolates the serotype was not identified. The percentage of non-O157 STEC cases has been increasing since 2014 possibly due to changes in lab methods and screening all submitted fecal samples for STEC infection, according to the report.
Thirty cases of listeriosis with two deaths were reported compared to 21 infections in 2017. All patients were hospitalized but there were no Listeria outbreaks. Between 1998 and 2018, the number of notifications has fluctuated between 17 in 1998 and 37 in 2016.
It was estimated by expert consultation that 25 of the 30 infections were due to foodborne transmission and 55 percent of these were because of eating ready-to-eat meats.
Rates for listeriosis were highest in the above 70 years age group for both the notifications and hospitalizations. The number of notifications was similar for females and males.
Norovirus, Yersinia and Shigella
Eight of 171 norovirus outbreaks and 362 of the 4,280 outbreak-associated cases were foodborne. Egg sandwiches served at a camp were the suspected source in one outbreak.
Between 2009 and 2018 the number of foodborne norovirus outbreaks ranged from eight in 2018 to 30 in 2009 and associated cases varied from 177 in 2013 to 552 in 2012.
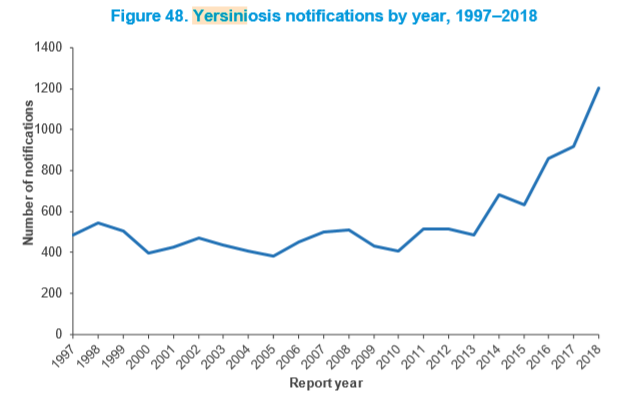
During 2018, 1,202 cases of yersiniosis and no deaths were reported in EpiSurv but 152 people needed hospital treatment. In 2017, 917 yersinia infections were recorded. It has been estimated by experts that 718 of the 1,202 cases were due to foodborne transmission and 70 percent are because of consuming pork.
One outbreak involving two people was linked to pork brawn. Between 2009 and 2018, there were three or less outbreaks each year with associated cases ranging from two to 232 in 2014.
One Shigella outbreak with three infections was thought to be foodborne. The food vehicle was unknown but suspected to be something eaten overseas. The number of foodborne shigellosis outbreaks ranged between zero and five from 2009 to 2018 with two and 39 associated cases.
One foodborne Staphylococcus aureus outbreak was reported with nine cases. The food source was unknown but it came from a restaurant, café or bakery. The number of outbreaks between 2009 and 2018 ranged from zero to two with between two and 14 cases.
Clostridium perfringens, Hepatitis A and fish poisoning
There was one Clostridium perfringens outbreak involving 21 people caused by a pork mince meal with rice and vegetables prepared at home. Between 2009 and 2018, the number of foodborne outbreaks ranged from one in 2016 and 2018 to nine in 2013. The most infections occurred in 2013 with 208 cases.
Three outbreaks caused by hepatitis A virus with eight cases were associated with a food source. The suspected infection source was shellfish for one outbreak and unknown for the other two incidents. Foodborne hepatitis A outbreaks are rare with only seven reported from 2009 to 2018.
Nine cases of histamine (scombroid) fish poisoning were reported during 2018. Two outbreaks involved five cases, two of whom needed hospital treatment. Tuna fish was suspected in one outbreak. Between 2009 and 2018 the number of histamine fish poisoning outbreaks each year ranged from one to four except for 2015, which had none.
Three cases of toxic shellfish poisoning but no deaths were reported although two had to be hospitalized. The toxin type was not specified in any case. All three were adults aged between 20 and 49 and had eaten recreationally collected seafood. Two were male and one female. Two were of Māori ethnicity and one was European or other.
(To sign up for a free subscription to Food Safety News, click here.)








