The number of Shiga toxin-producing E. coli infections in Europe jumped last year while the increasing trend of Listeria cases continued, according to an annual report on zoonoses.
The European Food Safety Authority (EFSA) and European Centre for Disease Prevention and Control (ECDC) analysis also revealed a slight rise in Salmonella and Campylobacter. For information on foodborne outbreaks click here for Food Safety News coverage in a related story.
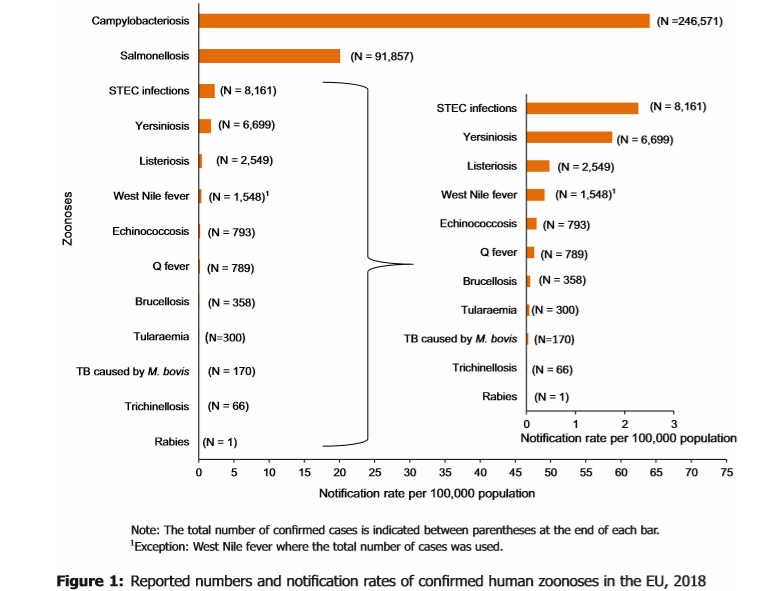
Shiga toxin-producing E. coli (STEC) became the third most common cause of foodborne disease replacing yersiniosis with a 37 percent increase on 2017. ECDC and EFSA said this may be partly explained by growing use of new laboratory technologies, making detecting sporadic cases easier.
The most commonly reported zoonoses were campylobacteriosis and salmonellosis. The EU trend for confirmed cases of these two diseases was stable during 2014 to 2018. Last year campylobacteriosis was top, as it has been since 2005, representing almost 70 percent of cases.
Campylobacteriosis caused almost 21,000 people to be hospitalized and 60 deaths, more than 16,500 people needed hospital treatment and 119 died due to Salmonellosis, STEC infections were responsible for 1,151 hospitalizations and 11 deaths, yersiniosis for 519 hospitalizations and three deaths and 1,049 people needed hospital treatment and 229 died due to listeriosis.
Impact of Campylobacter process hygiene criterion
The total of confirmed cases of campylobacteriosis was 246,571 compared to 246,194 in 2017. The highest hospitalization rates were in Latvia, Poland, Romania and the U.K.
The top country-specific notification rates were the Czech Republic, Slovakia, Luxembourg and United Kingdom. The lowest were in Bulgaria, Cyprus, Greece, Latvia, Poland, Portugal and Romania.
Among 15,210 travel-associated cases with known country of infection, most were from Spain, Greece and France. Thailand, Turkey and Morocco were most often reported as probable country of infection outside the EU. Highest contamination levels were in fresh meat from broilers followed by fresh meat from turkeys.
Austria, Czech Republic, Estonia, France, Hungary, Ireland, Italy, Latvia, Malta, Poland, Slovakia, Slovenia and Spain had significantly increasing trends between 2009 and 2018 while Cyprus and the Netherlands reported decreasing trends in this period.
Ten nations reported data collected as part of the Campylobacter process hygiene criterion in force since January 2018, which are about neck skins from broiler carcasses taken at slaughterhouses. Reporting of official sample results by authorities becomes mandatory from 2020.
One in five samples with quantified results were above 1,000 colony forming units (CFU) per gram. Of the 3,746 neck skin samples from chilled broiler carcasses, 34.6 percent tested positive. Bulgaria, Cyprus, Denmark, Estonia, France, Poland, Romania and Spain provided quantified results and 18.4 percent of 2,403 tested samples exceeded 1,000 CFU/g.
Salmonella decline levels off
In total, 94,203 salmonellosis cases were reported by 28 EU countries in 2018 with confirmed infections at 91,857 compared to 91,590 in 2017.
The highest notification rates last year were by Slovakia and Czech Republic, while the lowest came from Cyprus, Greece, Italy and Portugal.
Most confirmed salmonellosis cases were acquired in the EU. Salmonella Enteritidis increased in 2015 to 2018 in cases acquired within the EU. Among 8,047 travel-associated cases, Thailand, Egypt and India were the most frequently reported destinations with Spain and Greece the top places inside the EU.
Cyprus, Denmark, Finland, Germany, Hungary, Italy, Lithuania and Sweden had decreasing trends from 2009 to 2018. An increase was seen in France, Portugal, Slovakia and Spain in 2014 to 2018 but the rise in Spain was partly due to improved surveillance. The highest proportions of hospitalized cases were in Cyprus, Greece, Lithuania, Poland and the U.K. The latter country also reported 57 deaths.
Data by serovar
As in previous years, the three most common Salmonella serovars were Enteritidis, Typhimurium and monophasic Typhimurium (1,4,[5],12:i:-), accounting for almost 80 percent of cases acquired in the EU.
The proportion of these serovars was the same as 2017, as well as Infantis, which was the fourth most common. The serovar in fifth, Newport, increased by 18 percent versus 2017. Salmonella Coeln rose by 218.7 percent on 2016. Salmonella Braenderup entered the top 20 last year and replaced Kottbus.
The highest prevalence of Salmonella-positive single samples from official controls by authorities was poultry meat and minced meat and meat preparations intended to be cooked, irrespective of the species. Prevalence of Salmonella in egg products was negligible, according to monitoring data.
Of 27 reporting member states, 16 met all Salmonella reduction targets for poultry, whereas 11 failed at least one. The EU flock prevalence of target Salmonella serovars in breeding hens, laying hens, broilers and fattening turkeys decreased in recent years but stalled in breeding turkeys.
For Italy, Netherlands, Poland and Spain, the proportion of positives based on official controls was significantly higher than that from self-monitoring for pig carcasses. Considering all Salmonella monitoring data from pig carcasses sent by 17 countries, the proportion of Salmonella-positive single samples from carcasses based on official controls was 2.69 percent of 28,246 samples versus that based on self-monitoring at 1.57 percent of 93,633 samples.
Significantly lower proportions of Salmonella positive turkey and broiler flocks were reported in sampling by food companies in self-monitoring than by authorities in official controls.
STEC moves into third
Shiga toxin-producing E. coli infections were the third most commonly reported zoonosis in Europe and increased strongly in 2018. Last year, 8,314 STEC infections and 8,161 confirmed cases were reported compared to 5,958 in 2017.
The highest country-specific notification rates were in Ireland, Sweden, Malta and Denmark. Bulgaria, Cyprus, Greece, Lithuania, Poland and Romania had the lowest. The highest proportions of hospitalized cases were in Estonia, Greece, Latvia, Italy, Luxembourg, Poland and Slovakia.
Most STEC cases reported were infected in EU. Among 1,027 travel-associated cases, Turkey was most often reported as probable country of infection, followed by Egypt, Spain, Morocco and Greece.
In 2009 to 2018, a significantly increasing trend was observed in Austria, Denmark, Finland, France, Ireland, Italy, Slovenia and Sweden. No country had decreasing trends in this period.
E. coli O157 and O26 increase
The most common serogroup was O157, accounting for 34.5 percent of cases with known serogroup. Its proportion has been decreasing from 2012 to 2017 but increased by 29 percent in 2018. The second most common serogroup O26 increased by 32 percent. They represented more than half of the total confirmed cases with known serogroups in 2018.
They were followed by serogroups O103, O91, O146, O145 and O128. Two new serogroups (O5 and O174) were added to and O63 was dropped from the top 20 list in 2018.
A total of 411 cases of hemolytic uremic syndrome (HUS) were recorded, which was about the same as 2017. Most HUS patients were in the youngest age groups from 0 to 4 years (265 cases) to 5 to 14 years (82 cases). The top serogroups were O26, O157, O145, O80 and O111.
The most contaminated food categories were of animal origin. The small ruminants’ meat, from wild and farmed animals, presented the highest values (17.8 percent for deer and 10.9 percent for sheep and goat meat).
Raw cow’s milk was the second category most contaminated with STEC with less than 6 percent of samples positive. Fresh bovine meat and dairy products other than raw milk displayed 3.4 percent and 0.7 percent contamination rates.
Listeria continues to rise
Confirmed listeriosis cases further increased in 2018, despite Listeria rarely exceeding the EU food safety limit tested in ready-to-eat food.
Listeriosis was the most severe zoonoses with the highest hospitalization and case-fatality rate. One of every six confirmed cases were fatal. Long-term invasive listeriosis has shown a significant increasing trend since EU surveillance started in 2008.
In 2018, 28 countries reported 2,549 confirmed invasive cases of listeriosis compared to 2,479 in 2017. Listeria infections were mostly in the age group over 64 years and particularly in those over 84 years old.
Highest notification rates were for Estonia, Finland, Sweden and Denmark. The lowest were reported by Bulgaria, Croatia, Cyprus and Romania.
Belgium, Estonia, Finland, France, Germany, Greece, Hungary, Ireland, Italy, Netherlands, Poland, Romania, Slovenia and Spain had a significantly increasing trend of confirmed listeriosis cases since 2009. No country had significantly decreasing trends between 2009 and 2018. Poland reported the most fatal cases with 56 followed by France with 42.
Listeria monocytogenes occurrence varied according to the RTE food category and ranged from 0.09 percent for hard cheeses made from pasteurized milk up to 3.1 percent for RTE bovine meat.
EFSA has been told by the European Commission to issue a scientific opinion on the public health risk posed by Listeria monocytogenes, and possibly other pathogens, that may contaminate fruit, vegetables and herbs that are processed before being put on the market frozen. The work is due for adoption by the BIOHAZ panel in March 2020.
Yersinia, Brucella and Trichinella
Yersiniosis was the fourth most frequently reported infection with a stable trend in 2014 to 2018.
In 2018, 370 brucellosis cases, of which 358 were confirmed, were reported compared to 378 in 2017. One death was recorded by Spain in 2018.
Greece, Italy, Portugal and Spain are not officially brucellosis free in cattle, sheep or goats and accounted for 69.8 percent of all confirmed cases in 2018. Italy, Portugal and Spain had decreasing trends from 2009 to 2018. Foodborne exposure is normally limited to people consuming unpasteurized milk, dairy products or undercooked meat from countries where brucellosis in animals is endemic.
Among 58 travel-associated cases, the most common destinations outside the EU were Turkey, Iraq, Albania and Bosnia and Herzegovina. Romania and Bulgaria were the most common for travel-related infection within the EU.
In 2018, 85 trichinellosis cases, including 66 confirmed, were reported compared to 168 in 2017. Bulgaria recorded the highest notification rate, followed by Romania. The two countries accounted for 83.3 percent of all confirmed cases at EU level.
Four outbreaks were reported in Bulgaria with 50 people sick despite the absence of domestic pigs reported to be positive for Trichinella infection. In contrast, Croatia reported no human cases, whereas 134 domestic pigs were found to be positive. Romania accounted for the most positive domestic pigs followed by Croatia, Poland, Italy, Spain and France.
About 200 million pigs were tested for Trichinella in 2018, out of about 246 million reared pigs in the EU, with only 322 positive animals, about 1.3 per million reared pigs.
(To sign up for a free subscription to Food Safety News, click here.)








