Campylobacter, Salmonella and non-O157 Shiga toxin producing E. coli (STEC) cases increased in the United Kingdom in 2017, according to a report.
The U.K. Zoonoses Report found Listeria and STEC O157 cases declined. Zoonoses are diseases that can be transmitted from animals to humans. Campylobacter remained the most commonly reported human gastrointestinal pathogen and cases increased in 2017 after a decline over the previous two years.
A total of 63,946 cases were reported compared to 58,938 in 2016 and 63,201 in 2015. The reporting rate increased from 89.8 per 100,000 population in 2016 to 96.8 per 100,000 in 2017. This rise was seen in each of the U.K. countries. Northern Ireland continues to report rates lower than the others (76 cases per 100,000 population) but reasons for this are unknown.
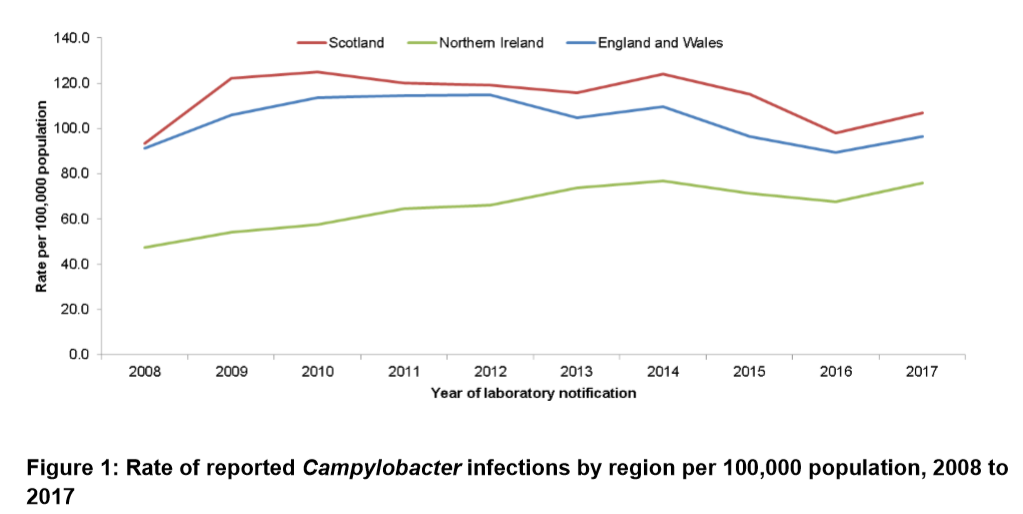
There were nine foodborne outbreaks of campylobacteriosis in the U.K., compared to eight in 2016. Seven were associated with consumption of poultry products, of which six were chicken or duck liver parfait or pate. Two outbreaks were linked to unpasteurized, raw milk and one Campylobacter jejuni outbreak affected 69 cases in England linked to a product made from raw milk.
Non-O157, STEC O157 and raw milk
The burden of disease because of non-O157 STEC is underestimated, according to the report, but labs introducing polymerase chain reaction (PCR) to directly find Shiga toxin genes has improved detection of serogroups other than O157.
In 2017, there were 589 laboratory confirmed cases of non-O157 STEC — 384 in England, one in Wales, 59 in Scotland and 145 in Northern Ireland — which represents a steady increase from the 59 cases in 2012. Serogroup O26 is the most common in the U.K. after O157, followed by O91, O146 and O103.
Meanwhile, there were 775 lab confirmed human cases of STEC O157 — 563 in England and Wales, 167 in Scotland, and 45 in Northern Ireland — compared to 959 the year before.
Incidence of STEC O157 decreased in all countries compared to 2016. The reporting rate for the U.K. overall is the lowest it has been in the last 10 years and follows a year on year decline in England since 2015. Scotland has recorded the highest rates of infection since 2008, except in 2012 when a large outbreak occurred in Northern Ireland.
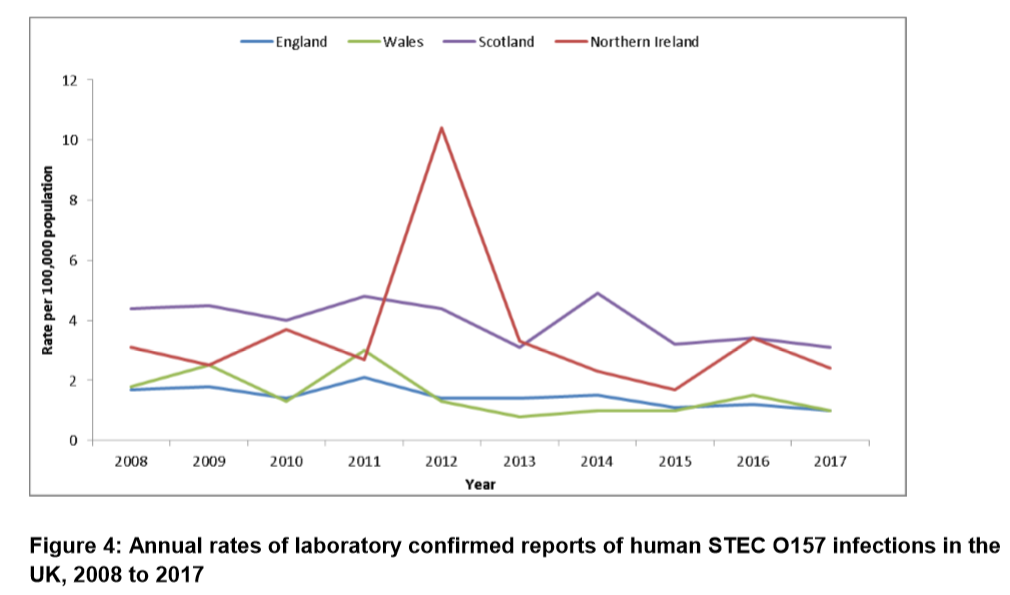
A total of 10 outbreaks were reported in 2017. Most were small, with a range of three to 17 people affected. Seven involved STEC O157 and three non-O157 — O26, O145 and O55. No common source of infection was determined for any of the non-O157 outbreaks.
STEC O157 outbreaks included two linked to raw drinking milk and burgers, one associated with a paddling pool, one nursery school outbreak where source of infection was unknown, one linked to raw pet food, and two with no known source of infection.
The O26 outbreak in August 2017 included two cases in Scotland and one in England. A national cluster of STEC serogroup O145 in September 2017 involved four infections from England and one from Scotland. An outbreak of STEC O55 in the South of England was a reoccurrence of incidents previously identified and investigated in 2014 to 2016.
The year saw the first STEC outbreak associated with raw drinking milk (RDM) in England and Wales since one in 2014 affecting nine cases. The STEC O157 phage type 21/28 stx2 outbreak was in autumn 2017 in the South of England. Investigations identified seven confirmed cases and three people developed Hemolytic Uremic Syndrome (HUS). Three more cases were notified following the recall, two of whom had drunk raw milk from the farm after the recall.
In Wales, a child infected with STEC who drank RDM died. Meanwhile, there were three outbreaks of Campylobacter affecting 27 people and Salmonella Dublin affected one person. There has been a rise in registered RDM producers in the UK with 168 in January 2018 compared to 108 in April 2014.
Salmonella cases pass 10,000
Slightly more than 10,000 cases of laboratory confirmed salmonellosis were reported in 2017. It is the first time since 2009 that more than 10,000 cases had been reported and continues the streak of a rise in infections every year since 2014.
Salmonella Enteritidis remained the most commonly reported serovar, accounting for 27 percent of cases.
Salmonella Typhimurium including monophasic strains was the second most common serovar, comprising 21 percent of cases, and increased 10 percent from 2016. This was due to a rise in cases in England; decreases were seen in other U.K. countries. Other common serovars were Newport, Infantis, Agona, Stanley, Java and Kentucky.
Thirteen foodborne outbreaks were reported compared to 12 in 2016. Two were caused by Salmonella Enteritidis, five by Salmonella Typhimurium and others by Salmonella Adjame, Salmonella Agona, Salmonella Chester, Salmonella Give, Salmonella Infantis and Salmonella Stanley. Eggs were implicated in two Salmonella Enteritidis outbreaks. Pork products were implicated in two others, both monophasic Salmonella Typhimurium.
Lowest Listeria count for a decade
There were 153 cases of listeriosis, a decrease compared to 202 infections in 2016, and the lowest total in the past 10 years. Of the cases in 2017, 44 percent were female, and 17 percent were associated with pregnancy.
The use of whole genome sequencing (WGS) for microbiological typing of Listeria isolates has led to an increased detection of linked cases, often over a prolonged time period due to the long-term persistence of Listeria in food premises. There were four incidents of listeriosis investigated and three comprised isolates spanning 2013 to 2017.
One outbreak was associated with a cooked chicken producer, one with a sandwich producer and for two the source of infection was unknown. Two incidents were investigated where a single case was microbiologically linked to one or more positive food samples through WGS analysis; one involving hospital sandwiches and the other a raw cheese product. A listeriosis death was reported in 2017 where the same strain was detected in a cheese product and the patient.
Hepatitis E and Cryptosporidium figures
Reports of hepatitis E virus (HEV) infections which have increased steadily for more than 10 years, finally dropped in 2017.
The downward trend across the U.K. saw 912 cases reported in England and Wales compared to 1,243 in 2016, 170 in Scotland versus 205 in 2016 and 10 compared to 18 in 2016 in Northern Ireland.
Factors behind this are unclear but may reflect the changing level of exposure to the virus via the food chain possibly influenced by changes in animal husbandry, farming practices, food processing and meat importation.
In developed countries HEV genotype 3 is the indigenous genotype and is transmitted mainly through ingestion of undercooked products from infected animals. Most cases are sporadic, however outbreaks have followed consumption of undercooked pork or deer meat, or uncooked shellfish.
The number of cryptosporidiosis cases was 5,052, a decrease of 25 percent compared to 2016. However, numbers were elevated in 2015 and 2016 because of an increase in Cryptosporidium hominis cases among people who had traveled to Spain and an outbreak of Cryptosporidium parvum linked to food from coffee shops.
(To sign up for a free subscription to Food Safety News, click here.)








