Shiga toxin producing E. coli (STEC) infections are at the lowest level since 2009, according to Dutch surveillance statistics.
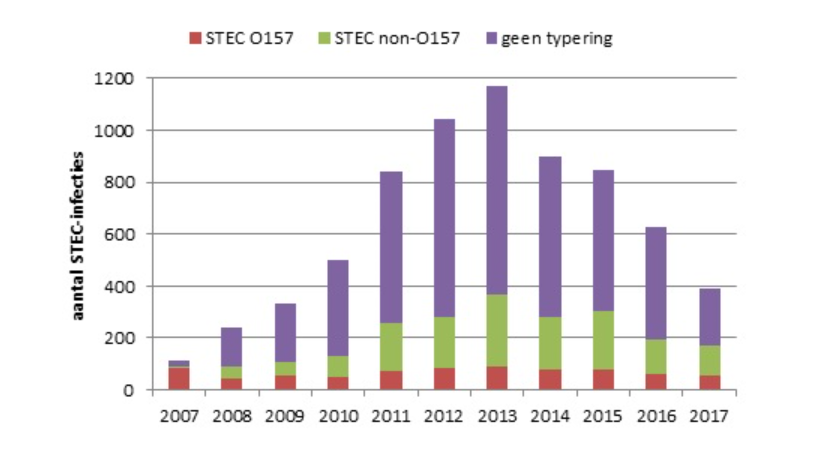
In 2017, 393 patients with STEC infection were reported, compared with more than 600 in 2016. Some of this decline is likely because of a change in reporting criteria from July 2016. Of the 393 patients, 58 had a confirmed STEC O157 infection and 114 a non-O157 STEC infection. The isolate could not be confirmed as STEC in 47 cases and no isolate was submitted for 174 patients.
Data was compiled by researchers from the Dutch National Institute for Public Health and the Environment (RIVM) and Netherlands Food and Consumer Product Safety Authority (NVWA).
The findings follow surveillance statistics on Salmonella which showed the Netherlands had one of the lowest incident rates in Europe.
For 55 of the 58 STEC O157 patients where the isolate was available, slightly more than half contained both Shiga toxin (stx) genes, 46 percent had only the stx2 gene, and one isolate had only the stx1 gene. Of the 107 available STEC non-O157 isolates, 42 contained only the stx1 gene, 47 only the stx2 gene and 18 isolates had both.
STEC O157 remains the leading cause of E. coli infections in the Netherlands, followed by STEC O26, STEC O103 and STEC O146. A total of 37 different O-groups were found.
Since non-O157 STEC has been included in Dutch surveillance, E. coli O26 has been in the top three most common O-types every year. However, E. coli O157 remains the most important, both in number and severity with hospitalization seen more often with it than other O-types.
Hemolytic uremic syndrome (HUS) was reported for 12 patients, including four children from 1 to 4 years old and eight adults from 33 to 84 years old. Two adults died from STEC infection: an 81-year-old male and an 83-year-old female, both with an untyped STEC. HUS is a type of kidney failure that can occur among people of any age but is most common in children younger than five and older adults.
For typed STEC infections, 17 to 18 percent were contracted abroad. For untyped infections that figure was 28 percent.
Most STEC O157 infections, 60 percent, were seen in the months of June through August. This trend was less strong (41 percent) but the same for STEC non-O157 infections. The peak of non-typed STEC infections was from July to September, with 43 percent of cases reported during those months.
Almost all patients with O157, STEC non-O157, or other/not typed infections said they ate meat before becoming ill, with 88 to 100 percent in that category. Researchers reported raw milk appeared to have been drunk more often by STEC O157 patients, representing 21 percent of patients, than by the other two groups, which were reported at 7 percent. STEC O157 patients also had more contact with pets (72 percent) than the other groups (42-53 percent).
WGS was used for cluster detection for the first time for all available isolates in 2017. The switch from PFGE to WGS for STEC O157 infections did not lead to major changes in detection of clusters as the number and sizes were comparable. However, WGS results were available quicker than PFGE and they could be compared easier with findings from other institutes and countries.
Last year was the first full year following introduction of new reporting criteria in July 2016. The focus of STEC surveillance is now on acute infections. As expected by tightening criteria, the decrease in reported STEC infections continued, but the average amount of information on patients increased.
Following a complaint or suspected food source of infection, six samples were tested for STEC by the NVWA. STEC was shown in one sample but it was not possible to show a match with the infection because no human isolate was available.
A total of 56 isolates were found in food, with 31 different O-groups detected. E. coli O146:H21 was the most commonly found at eight times.
In 2017, NVWA investigated presence of STEC in food in 23 projects with the focus on retail meat. The highest prevalence was in fresh meat from small ruminants as in 18 of 196 samples a STEC isolate was found. Monitoring at retail from small ruminants showed an even higher prevalence with five isolates in 29 samples. In veal, the rate was also high with 16 isolates in 236 samples.
In monitoring on fish products, mussels, oysters and live bivalves an isolate was only found in one sample of live bivalves. For vegetables and herbs, two samples were positive in raw vegetables.
(To sign up for a free subscription to Food Safety News, click here.)









