E. coli infections continued to climb in Switzerland in 2019, according to the country’s surveillance report on zoonoses and outbreaks of food poisoning.
The most common zoonoses were again campylobacteriosis and salmonellosis. There were about 7,000 cases of campylobacteriosis and 1,500 of salmonellosis, but the actual number is likely to be higher, according to the Federal Food Safety and Veterinary Office (FSVO).
Food and waterborne outbreaks almost doubled from 12 in 2018 to 23 in 2019, the highest level in the past decade. In total, more than 331 people fell ill and at least six were hospitalized.
Continued E. coli rise
The year was marked by a further increase in Shiga toxin-producing E. coli (STEC) to 993 confirmed cases from 822 in 2018. The rate is the highest recorded since introducing reporting obligations in 1999.
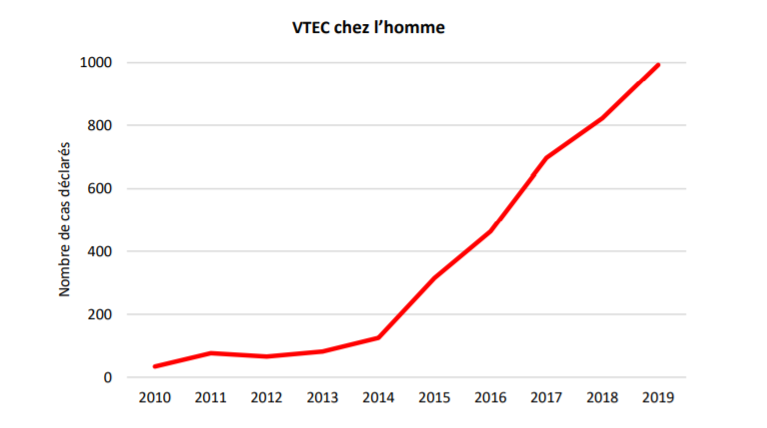
The main cause of this rise is probably due to new analytical methods as labs are performing more tests for STEC, which allows more cases to be detected. The number of HUS cases remaining practically constant throughout the years backs up this hypothesis, according to FSVO, which is also known in Italian as USAV, French as OSAV and German as BLV.
As in 2018, most cases were recorded in the third quarter. With the exception of children under 5, women were slightly more affected than men regardless of age. A possible country of exposure was noted in 662 cases, Switzerland was mentioned in 399 cases.
With 20 cases of hemolytic uremic syndrome (HUS) in 2019, there was a slight decrease compared to 23 the previous year. Eight children younger than 5 and six people 65 and older were mostly affected.
Campylobacter, Salmonella and Listeria
In 2019, campylobacteriosis remained the most frequently recorded infection. A total of 7,223 cases confirmed by laboratory diagnosis were reported which was a slight decrease compared to 7,675 in the previous year.
A first increase was noted in summer. The peak was reached in July and August, with 1,817 cases. As in previous years, a second short-lived rise was recorded during the holiday season linked to the Swiss version of Chinese fondue.
As part of self-monitoring by the poultry sector, 1,482 analyzes were carried out on chicken and turkey meat in 2019. Of these, 323 tested positive for Campylobacter spp. Campylobacter was between 1,000 and 10,000 colony forming units per gram for 38 of 390 chicken carcass samples analyzed and it was higher than 10,000 in 17 samples. If rates frequently exceed 1,000 CFU/g the slaughterhouse must take measures to achieve a reduction such as improving hygiene and monitoring of process controls.
The second most frequent zoonosis in Switzerland was salmonellosis. In 2019, 1,547 cases confirmed by lab diagnosis were reported which was a slight increase compared to 1,467 in 2018. The most frequently reported serovars are Salmonella Enteritidis, followed by Typhimurium and its monophasic variant 1,4,[5],12:i:-.
As part of self controls by the poultry sector, 3,216 analyzes were done on chicken and turkey meat in 2019. In total, 16 were positive: five cases each of Salmonella Albany and Enteritidis, four of Salmonella Infantis, and one each of Salmonella Typhimurium and Heidelberg.
In 2019, 36 cases of listeriosis confirmed by lab diagnosis were reported compared to 42 in 2018. As in previous years, the highest reporting rate was in the older than 65 age group. Serotypes 4b and 1/2a were the most frequently detected.
More than 1,000 cheese and 202 environmental samples were tested for Listeria and while Listeria monocytogenes was not detected other types of Listeria were found in 11 samples. Swiss meat products were tested as part of a project commissioned by FSVO. Two hundred samples were analyzed and Listeria monocytogenes was found three times but did not exceed the limit of 100 CFU/g.
More outbreaks but total still low
Foodborne infections have been rare in Switzerland for several years with 23 incidents reported for 2019. This figure, although double the previous year, remains low compared to other countries.
For five people with hepatitis E, interviews with patients suggested pork as the cause of disease. No source was suspected in five Salmonella outbreaks. Salmonella Napoli affected 50 people, Salmonella Munchen left 38 ill, Salmonella Derby sickened 23, seven were ill from Salmonella Hvittingfoss and eight because of Salmonella Bovismorbificans.
The infectious agent causing outbreaks could only be determined in two of 23 incidents. One involved Campylobacter and the other norovirus along with E. coli and enterococci.
Two days after having a meal at a restaurant, a family of three fell ill. Campylobacter was detected in stools of patients. Mozzarella-stuffed chicken breast was suspected, but analysis could not be performed as no sample was still available. An investigation at the restaurant showed meat was likely undercooked.
During a summer camp, 45 children and eight adults in two cabins fell ill. Norovirus type I was detected in the stool of a patient. As water was suspected, analyzes found type I and type II norovirus as well as E. coli and enterococci.
In other investigations, two people fell ill possibly from histamine poisoning in tuna that was stored incorrectly. Six people became sick one day after eating a ham sandwich from a bakery where norovirus was found in the stool of an employee. Finally, the chef of a restaurant, suffering from nausea and diarrhea, still came to work. Following a meal served the same evening to 25 guests, 15 people presented similar symptoms and a cook in the restaurant also became ill.
(To sign up for a free subscription to Food Safety News, click here.)








