Belgium has recorded the highest number of foodborne outbreaks in a year since recordkeeping began.
This past year, 571 outbreaks were reported to the National Reference Laboratory for Foodborne Outbreaks (LNR-TIA). A total of 2,457 people fell ill and 28 were hospitalized.
Data on outbreaks have been collected by Sciensano, the Belgian Institute for Health, since 1999. From 1999 to 2010, 39 to 116 outbreaks were reported each year, but this number doubled in 2011 to 281. There were an average of 336 outbreaks per year between 2011 and 2016. Almost 400 outbreaks were recorded in 2018.
The number of patients varied from 531 to 2,457 between 1999 and 2019, with a peak of more than 4,000 in 2010 following a water-related outbreak. Despite the amount of patients going up, the hospitalizations figure has gone down, indicating milder outbreaks are being detected.
Unknowns in most outbreaks
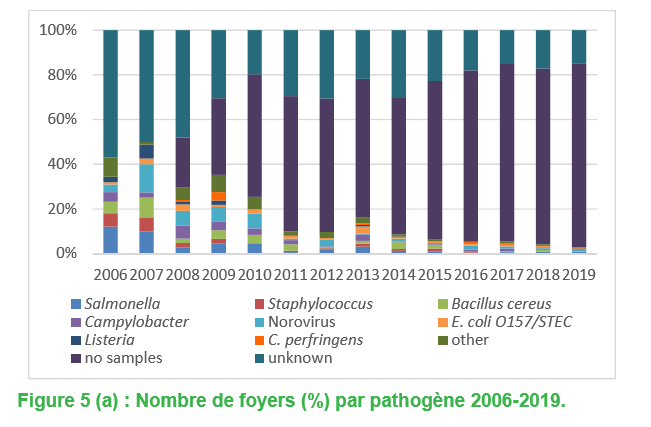
Salmonella was the most commonly reported agent causing an outbreak of foodborne illness in 2019 and made at least 216 people sick. Norovirus was second and made at least 41 people sick. Clostridium perfringens, Listeria monocytogenes, Campylobacter, Bacillus cereus and E. coli are among other germs identified.
No samples were received in 1,500 of the 2,457 illnesses and the agent was unknown for 600 cases. The cause behind 19 of the hospitalizations was also unknown. An unidentified agent caused 85 of the 571 outbreaks and no sample was received for 469 of them.
The report also covered Belgian infections as part of multi-country outbreaks such as Salmonella Poona linked to infant formula made at the Industrias Lacteas Asturianas SA (ILAS) factory in Anleo, Spain, and marketed by Sodilac under the Modilac brand, and Listeria from meat made by Offerman, a Ter Beke subsidiary in the Netherlands.
More than two thirds of the 571 outbreaks were caused by mixed foods. Meat products such as beef, pork, mutton and poultry were responsible for almost 13 percent of outbreaks. Fish products and crustaceans, shellfish and mollusks caused around 4 percent each of outbreaks.
The majority of outbreaks occurred in commercial establishments, such as restaurants, cafés or hotels and fast food chains or takeaways. Food delivered by catering companies to the workplace, establishments or at events was responsible for 0.9 percent, 1.2 percent and 0.7 percent of outbreaks, respectively. The number of incidents occurring at home was 15.6 percent.
Salmonella, Campylobacter, Listeria and E. coli
Five outbreaks of Salmonella were reported in 2019, and for two there was strong evidence contaminated food was the cause of infection. A total of 216 patients were reported and six had to be hospitalized.
One of these incidents led to 203 infections. The outbreak at a Belgian school was likely caused by eggs used to make a tartar sauce. Salmonella Enteritidis 3-12-5-5-1 was detected in human cases and food. Eggs came from a Spanish farm. France also identified 13 cases with isolation dates between May and October 2019.
Since 2005, Campylobacter has been the most reported intestinal pathogen and 7,051 cases were recorded in 2019. One outbreak involved two people with ice cream as the possible cause but food samples were negative.
In 2019, 67 listeriosis cases were reported compared with 74 in 2018. This past year Listeria monocytogenes was responsible for two outbreaks involving four people, and half of them had to be hospitalized. In the first outbreak, Listeria monocytogenes 1/2a was isolated from beef. In the second event, cheese was reported as a potential source of infection, but the pathogen was only detected in patients.
One outbreak of Enterohemorrhagic E. coli (EHEC), a subgroup of Shiga-toxin producing E. coli (STEC), was recorded with three cases and one person needed hospital treatment. A child developed hemolytic uremic syndrome (HUS). E. coli O26 stx2a eae was detected in the other child. The food source was likely raw beef consumed as carpaccio.
Bacillus cereus, norovirus, Clostridium perfringens and histamine
Arcobacter butzleri, considered an emerging pathogen in the food chain, was isolated from one of 40 sick wedding guests but not found in chicken legs, which were the suspected source of illness.
An outbreak of Bacillus cereus was associated with prepared spaghetti. In total, four people fell ill mainly suffering from nausea and vomiting. Two outbreaks were caused by Clostridium perfringens with 36 patients. The causative agent was detected in human samples but not in suspected foods.
In 2019, there were three norovirus outbreaks with detection of the virus in food and/or samples from patients and/or people who prepared the food, transmission having probably occurred via food.
One outbreak affected 26 people after eating sushi and oysters at a staff party. Norovirus GII was detected in the remaining oysters. In the other two incidents, involving 21 people, norovirus was only detected in patients or those who prepared the food.
Histamine was the source of one outbreak affecting nine people. Histamine concentrations of 52.9 and 80.5 milligrams per kilogram were detected in tuna leftovers.
(To sign up for a free subscription to Food Safety News, click here.)









