The numbers of people infected with E. coli and Listeria increased but there was a decrease for Salmonella and Campylobacter in Sweden in 2018.
The findings come from an annual report describing surveillance in the country during last year published by the National Veterinary Institute (SVA).
Campylobacter decline
A total of 8,132 cases of campylobacteriosis were reported in 2018 compared to 10,608 in 2017. Of the 2018 infections, 3,645 were domestic. Among these, the median age was 47 years with a range from 0 to 95 years old.
Like previous years, domestic incidence was highest in adults and more men (56 percent) than women were affected. Domestic incidence was lower in 2018 than previous years but the trend over a longer time period is increasing.
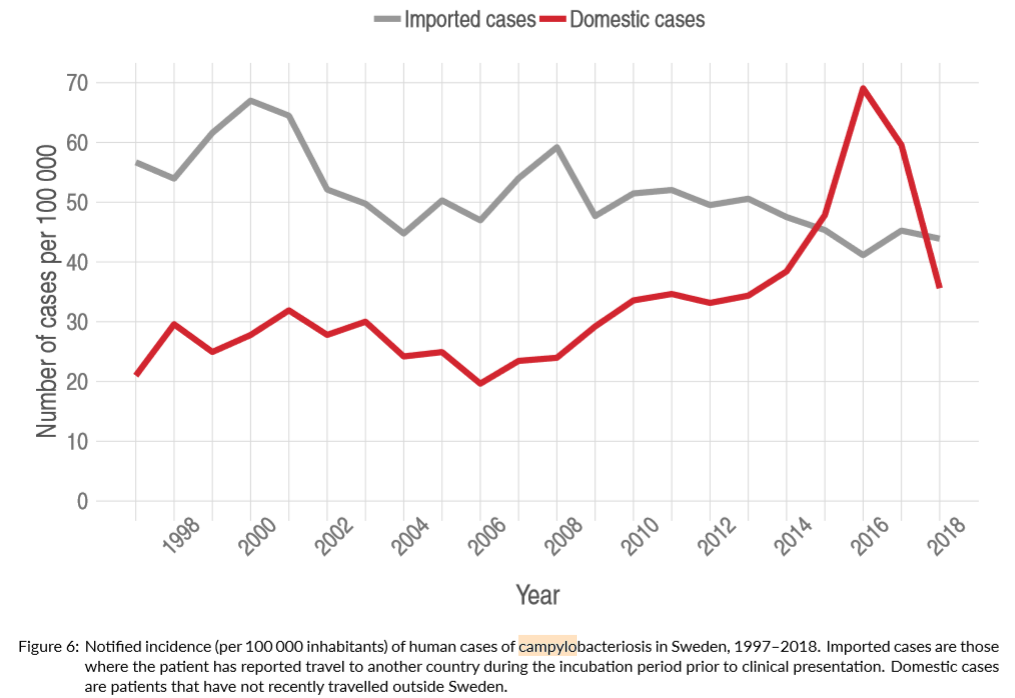
Most campylobacteriosis cases are considered sporadic but in recent years, several large outbreaks linked to domestically produced chicken have occurred. They show the importance of effective control and preventive measures in poultry production, according to the report.
In August 2018, a survey by the National Food Agency (Livsmedelsverket) collected 100 samples of fresh chicken meat at retail. Campylobacter was detected in 61 percent of 100 samples and levels exceeded 10 colony forming units per gram (cfu/g) in 25 percent of samples.
An outbreak in late autumn associated with domestic chicken meat and the high detection rate of Campylobacter in the survey on retail meat warrant stringent preventive measures, according to the report.
Listeria rises
Last year, 89 cases of listeriosis were reported, a minor increase on the 81 infections the year before and part of an increasing trend since 1983, which has also been seen in other EU countries.
The median age was 71 years and 57 percent were people were over 70 years old. Almost a third (29 percent) of reported cases died within one month of diagnosis. A total of 86 of the reported cases had Sweden as country of infection.
“The reasons for the increase remain unclear but are most likely related to a combination of factors such as an ageing population, a widespread use of immunosuppression medications and consumer preference changes to more ready to-eat foods,” according to the report.
In the past 10 years, 50 to 120 cases were reported annually. Outbreaks have been associated with vacuum-packaged fish, unpasteurized goat’s milk cheese, cold cuts, frozen corn and ready-to-eat foods.
During 2018, an outbreak was identified in the county of Västra Götaland. Seven cases had onset of disease between February and May. The outbreak strain was detected in ready-to-eat food from a local producer and products were recalled.
In 2018, 410 samples from different types of food were sampled by national and local authorities and analyzed for Listeria monocytogenes. It was detected in nine samples. Levels were quantified in seven of these and ranged from less than 10 cfu/g to 50cfu/g.
Salmonella infections drop
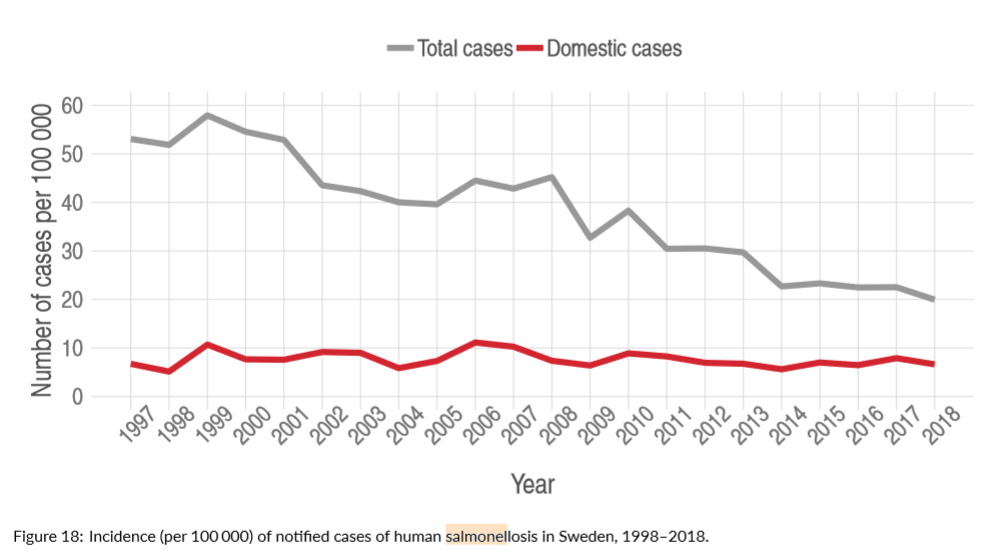
A total of 2,000 to 3,000 cases of salmonellosis are annually reported to the Public Health Agency of Sweden (Folkhälsomyndigheten). Most, 70 to 80 percent, are infected abroad but since 2008, a steep decrease in travel-associated cases has been noted, despite a rise in international travel.
In 2018, 2,040 cases of salmonellosis were reported, compared to 2,279 in 2017. Domestic cases decreased by 15 percent from 798 cases in 2017 to 677 in 2018. Among domestic cases, the median age was 42 years with a range of 0 to 99 years and the incidence was highest for persons over 80 years of age followed by children 1 to 4 years old.
The most common serovars from domestic cases were S. Enteritidis, S. Typhimurium followed by monophasic S. Typhimurium. Around 70 additional serovars were identified during 2018.
Two thirds, or 1,355, of the 2,040 cases were infected abroad. Of these, 18 percent were serotyped and S. Enteritidis was the most common serovar in 42 percent of the isolates typed. Thailand is the top country for travel associated salmonellosis, although the number of cases has decreased in past years.
Swab samples were taken from 5,879 pig carcasses, 3,272 cattle carcasses and neck skin samples from 2,780 poultry carcasses. Salmonella was detected in one pig carcass sample. At cutting plants, 5,173 samples of red meat and 1,118 of poultry meat were taken but Salmonella was not detected.
Seven domestic outbreaks of Salmonella were investigated during 2018 with 152 cases. The largest was caused by S. Bovismorbificans with 40 cases from 13 counties. No common source was found but beetroot sprouts were suspected. Early in 2018, a cluster of 17 cases with S. Mikawasima was identified and the same serovar was also detected in Denmark, Germany and the United Kingdom. An international outbreak investigation could not identify the source.
In 2018, Salmonella Typhimurium, MLVA profile 3-10-10-NA-211, was implicated in an outbreak with salami being the confirmed source of infection. In total, 18 cases were laboratory confirmed and the majority ate a specific type of truffle salami from Italy. The outbreak strain was detected in two opened packages of truffle salami.
During the last three years, salami has been implicated in five national Salmonella outbreaks in Sweden with 156 reported cases. In four of the investigations, the outbreak strain was isolated from suspected salami sausages.
E. coli elevation
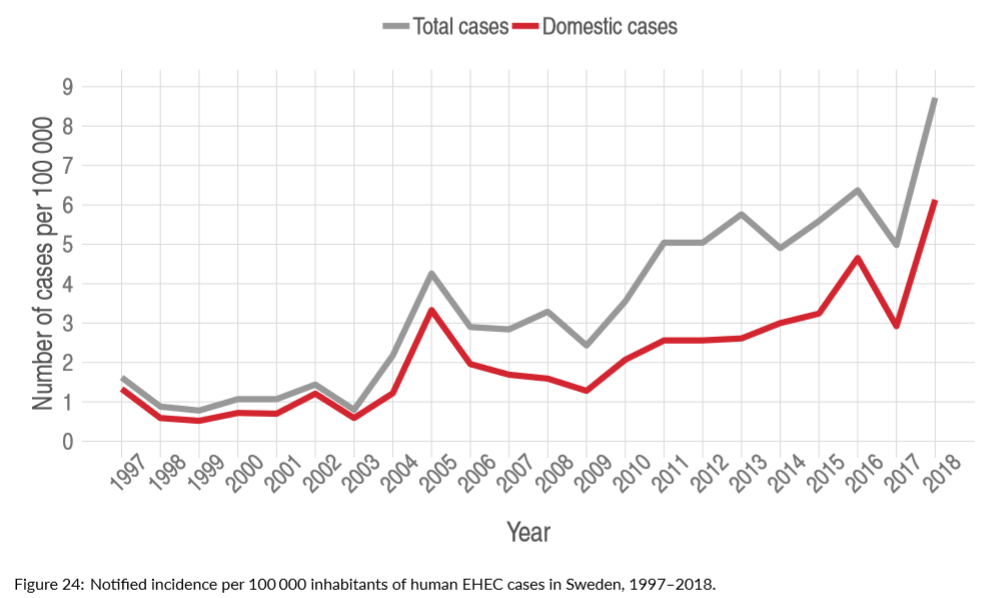
Since 2005, between 230 and 890 cases of STEC infections have been reported in Sweden annually, of which 50 to 80 percent were domestically acquired.
In 2018, 892 cases of Shiga toxin producing E. coli (STEC) were reported of which 627 were domestic compared to 504 and 296 domestic cases in 2017.
The domestic incidence was twice as high as the year before and over a longer period of time an increasing trend can be seen. The trend continued to rise, even without including cases from a large outbreak.
From autumn 2017 to spring 2018, a survey by the National Food Agency took 300 samples of lamb meat from retail and analyzed for STEC. It was detected in 35 percent of 300 samples. STEC was most often in lamb from Ireland, followed by Sweden and New Zealand. The most common serotype was STEC O91:H14.
STEC-associated hemolytic uremic syndrome (HUS) was reported in 40 cases of which 36 were domestically acquired. Most HUS cases were children under the age of 10. For 31 of them an isolate could be retrieved and serotyped.
Eighteen of the domestic HUS cases belonged to serotype O157:H7, clade 8, of which 14 belonged to a summer outbreak. In 67 percent of the domestic STEC cases, an isolate could be retrieved and serotyped. The most common serotypes were O157:H7, O26:H11, O121:H9 and O103:H2.
During the summer of 2018, one of the largest STEC outbreaks ever in Sweden occurred. A total of 116 cases were microbiologically or epidemiologically linked to it and 14 developed HUS. Cases were spread across the country but with some link to two restaurants and two public outdoor baths. The source of infection was not identified but is likely to have been foodborne since people fell ill in different parts of the country. Locally, it also seems infection was spread from person to person via outdoor bathing sites.
An outbreak of STEC O26:H1, stx1a occurred in late summer 2018 affecting 13 persons. The source of infection was not identified.
(To sign up for a free subscription to Food Safety News, click here.)









