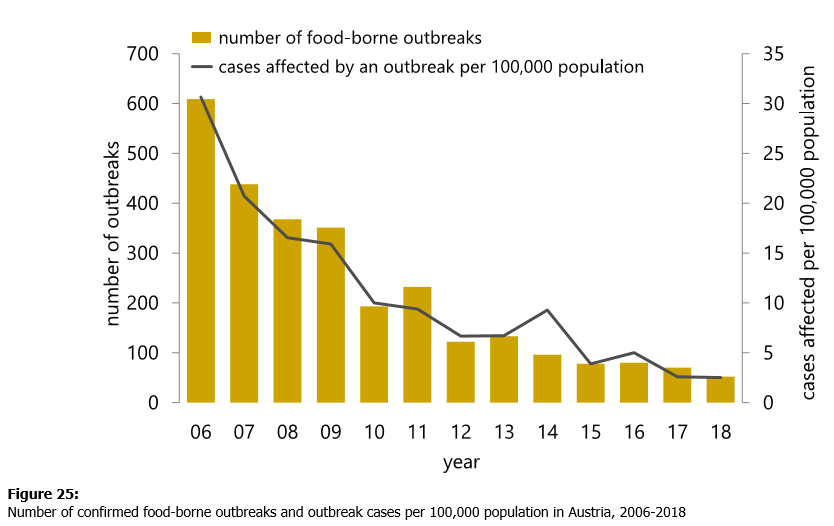
The number of foodborne outbreaks in Austria continues to decline with only 52 reported in 2018.
This figure was 69 in 2017, 80 in 2016 and 368 a decade ago, according to a report from the Federal Ministry for Labour, Social Affairs, Health and Consumer Protection (BMASGK) and Austrian Agency for Health and Food Safety (AGES).
In 2018, three-quarters of outbreaks were classed as household outbreaks. Eighteen, or more than one third, could be connected to stays abroad, compared with between 7 and 19 percent in previous years.
A total of 222 individuals were affected, nearly the same as the 227 people in 2017, but less than any year before. Fifty-eight people were hospitalized but no fatalities were reported, compared with 56 people needing hospital treatment and two deaths in 2017.
The most frequently detected agent was Campylobacter 24 times. Three outbreaks were caused by Shiga toxin-producing E. coli (STEC), two by norovirus and one each for Listeria monocytogenes and hepatitis A virus.
In STEC outbreaks, serotype O157:H7 and O103:HNM were detected as were both serotypes O91:HNM and O128:H not-typable in one incident. In the listeriosis outbreak, Listeria monocytogenes serotype 4b was typed, the one caused by hepatitis A virus had genotype IB SW 18-9763.
There has been a decrease in salmonellosis outbreaks of 95 percent from 454 to 21 between 2006 and 2018. Salmonella Enteritidis was the most frequent serovar with 15 outbreaks. Typhimurium caused four outbreaks and types Ibadan and Typhi were identified in incidents associated with travel abroad.
Foods identified as infection sources in strong-evidence outbreaks included egg products, meat products, chicken meat and such products, frozen strawberries and mixed foods.
This year, six people are part of an E. coli O157 outbreak, five are sick because of Listeria and 304 people were infected with Salmonella in eggs from Poland.
Campylobacter climbs
In 2018, there were 7,982 lab-confirmed campylobacteriosis cases officially reported. Compared with the 7,201 figure in 2017, incidence levels increased by 10.8 percent.
Campylobacter jejuni accounted for 88.4 percent of the specified 7,324 isolates, Campylobacter coli for 11.7 percent and in ten patients both species were detected.
Thermo tolerant Campylobacter was detected in 67 of 110 fresh poultry meat samples. Of these, 44 were found in 59 samples from fresh, raw chicken meat, in three of 11 samples of fresh turkey meat and in 20 of 40 samples of unspecified fresh poultry meat.
A seasonal incidence of campylobacteriosis reveals the fewest infections between November and April and the most from June to September. An almost identical picture is seen in isolation rates of thermo tolerant Campylobacter in slaughtered broiler flocks, with peak rates in summer months, suggesting higher contamination in fresh chicken at retail and pointing to this food as an important infection vehicle.
Salmonella in second
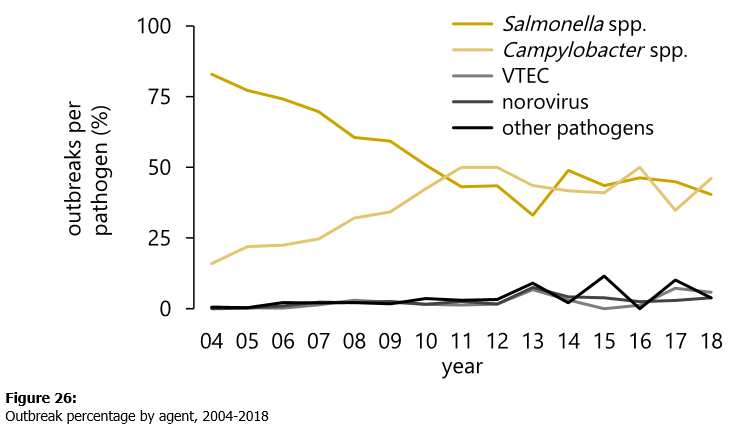
Salmonella was the second most common cause of bacterial food poisoning after Campylobacter.
In 2018, 1,533 lab-confirmed cases were reported to the Epidemiological Reporting System compared to 1,672 in 2017. The number of Salmonella Enteritidis cases declined to 723 last year and was below the 810 infections caused by all other serovars.
Salmonella Infantis, the most common serovar in broilers, and the monophasic variant of Salmonella Typhimurium have become increasingly important besides Enteritidis and Typhimurium.
Almost 5,000 samples were tested for Salmonella as part of the control and sample plan, as well as in targeted campaigns. Salmonella was identified in 68 samples, mainly Salmonella Infantis 54 times. It was found in 66 of 400 poultry meat samples.
Forty of 143 raw chicken meat samples tested positive for Salmonella, so did four of 18 raw chicken meat preparations and 22 of 139 raw poultry meat samples such as duck and goose. Salmonella was detected in one of 839 samples of mixed minced meat and one sample of foodstuffs intended for special nutritional uses.
Listeria records and continued STEC rise
A total of 27 cases of invasive listeriosis were notified and eight people died compared to 32 cases and six deaths in 2017. Two pregnancy-associated cases were identified last year, one premature birth and sepsis and one case of intrauterine death.
The risk of getting listeriosis was more than 12 times higher for people older than 65 than for younger people in 2018.
Last year, 2,887 food samples were tested and Listeria monocytogenes was found 72 times. This included in 46 of 672 meat samples, seven of 259 samples of fish and seafood, six of 517 samples of cheeses, 12 of 627 samples of ready-to-eat foodstuffs and one ready-to-eat salad with mayonnaise.
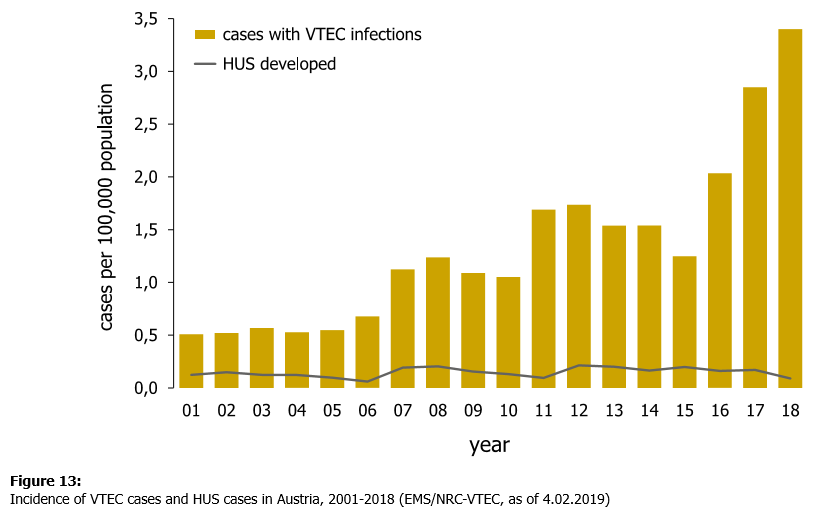
300 lab-confirmed STEC cases were notified which is almost a threefold increase compared to 2015 and up 50 from 2017. The rise can be traced to more samples from patients being tested.
The serious complication hemolytic uremic syndrome (HUS) occurred in eight cases, corresponding with the average in recent years. The most common serotype was STEC O157 with 45 cases.
Children from 0 to 4 years old were mostly affected with 30 percent of cases related to that age group.
Last year, 1,147 food samples were tested for STEC, of which 709 were meat. STEC were detected in 17 of 313 raw meat samples. One of 208 samples of ready-to-eat meat products was contaminated as were two of 237 tested sausages.
Typing of the 20 STEC-isolates revealed 11 serotypes. STEC O146 was isolated from three samples of fresh game meat and one fermented sausage. STEC O91 was detected in three samples of fresh meat.
Yersinia and Brucella
A total of 136 lab confirmed cases of yersiniosis were notified, an increase of 41 percent compared with the 95 cases in 2017.
Typing of Yersinia enterocolitica revealed serotype O:3 biovar 4 in 87 percent of cases, serotype O:9 biovar 2 in 12 percent and one isolate of serotype O:5,27 biovar 2 and one serotype O:9 biovar 3.
Yersiniosis mostly affected children below 5 years old. A strong rise of cases was seen in age groups 0 to 4, 5 to 14 and 15 to 24.
In 2018, seven lab-confirmed Brucella cases were documented. Five cases, four of which showed clinical symptoms, were associated with an outbreak of brucellosis at a dairy farm. Other cases were imported.
In June, brucellosis due to Brucella melitensis was confirmed at a large dairy farm in Upper Austria. It was not possible to clarify how Brucella was introduced into the holdings. Consumers were not at risk of acquiring it because milk delivered from that holding was pasteurized in a dairy plant prior to distribution.
(To sign up for a free subscription to Food Safety News, click here.)







