Antimicrobials used to treat diseases such as campylobacteriosis and salmonellosis are becoming less effective, according to a new research report.
The European Centre for Disease Prevention and Control (ECDC) and European Food Safety Authority (EFSA) report confirmed the rise in antibiotic resistance identified in previous years.
Data on antimicrobial resistance (AMR) in zoonotic and indicator bacteria in 2017, submitted by 28 EU member states, were analyzed by EFSA and ECDC. AMR data on food and food-producing animals specifically targeted fattening pigs and calves less than 1 year of age and their meat.
The agencies looked at antimicrobials used to treat diseases that can be transmitted between animals and humans, known as zoonoses. Infections can be acquired from animals, via environmental exposure, or through contaminated foodstuffs.
Vytenis Andriukaitis, EU Commissioner for Health and Food Safety, said the report should ring alarm bells.
“It shows that we are entering into a world where more and more common infections become difficult – or even sometimes impossible – to treat. However, ambitious national policies in some countries limiting antimicrobial use have led to a decrease of antimicrobial resistance,” he said.
“So before the alarm bells become a deafening siren, let’s make sure that we increasingly act all together, in every country and across the public health, animal health and environment sectors under the One Health approach umbrella.”
Prudent use of antimicrobials is essential to limiting the emergence and spread of antibiotic-resistant bacteria in humans and animals.
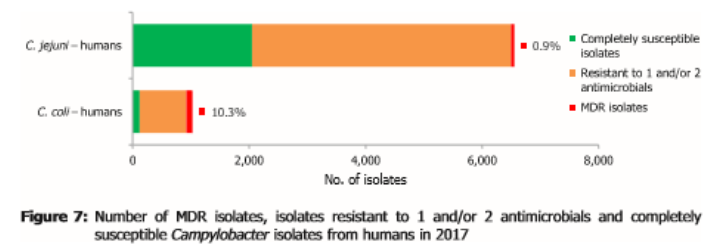
Resistance to fluoroquinolones such as ciprofloxacin is so high in Campylobacter in some countries that these antimicrobials no longer work to treat severe campylobacteriosis cases. In five countries, high to very high proportions of Campylobacter coli from humans were resistant to erythromycin, leaving few options for treatment of severe infections.
Very high to extremely high resistance levels to ciprofloxacin were reported in Campylobacter jejuni isolates from humans by all countries except Denmark, Iceland, Ireland, Norway and the United Kingdom.
Most countries reported that Salmonella in humans is increasingly resistant to fluoroquinolones. High proportions of isolates were resistant to ampicillin, sulfonamides and tetracyclines, but resistance to third-generation cephalosporins was uncommon.
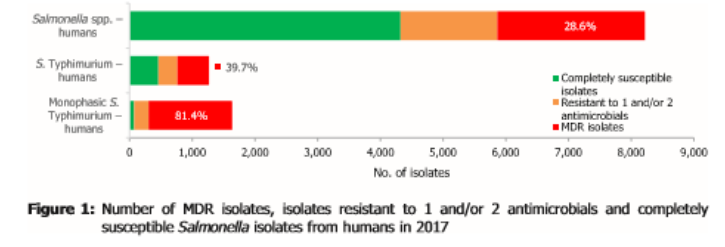
The proportion of Salmonella isolates resistant to clinically important antimicrobials ciprofloxacin (13 percent) and cefotaxime (1.9 percent) was relatively low. Resistance to last line antimicrobials, such as azithromycin and tigecycline, was low at 2.5 percent and 0.8 percent, respectively.
There were no Salmonella isolates recovered from carcasses of pigs and calves, fattening pigs and cattle which were resistant to carbapenems. In 2016 data, resistance was detected in poultry to this antibiotic which is not authorized for use in animals.
Multidrug resistance, which is resistance to three or more antimicrobials, is high in Salmonella in humans at 28.3 percent and animals, particularly Salmonella Typhimurium. Two isolates of Salmonella Typhimurium were resistant to eight of nine tested substances, only susceptible to meropenem.
Combined resistance to critically important antimicrobials was low to very low in Salmonella and Campylobacter from humans and animals, and in indicator E. coli from animals.
Mike Catchpole, ECDC’s chief scientist, said action on antimicrobial resistance is needed to keep antibiotics working.
“It’s particularly worrying when it comes to combined resistance: even low proportions mean that many thousands of patients across the EU have limited treatment options for severe infections,” he said.
Nineteen countries investigated almost 17,500 samples from meat from pigs collected at retail, fattening pigs collected at slaughter, meat from bovines collected at retail, and cattle less than 1 year old collected at slaughter. All samples were negative for carbapenemase-producing E. coli.
Among the nine serovars reported with extended-spectrum beta-lactamase (ESBL), the carriage was the highest in Salmonella Kentucky at 20.3 percent.
Meticillin-resistant Staphylococcus aureus (MRSA) was detected in meat from cattle, pigs or rabbits by four countries. MRSA is not generally considered to be transmitted by food. Resistance to important medical antimicrobials, vancomycin and linezolid, was not detected in MRSA isolates from meat, food-producing animals or following clinical investigations.
(To sign up for a free subscription to Food Safety News, click here.)








