Cattle in Scotland have a higher level of a certain subtype of E. coli O157 which causes more severe human infections, according to a report.
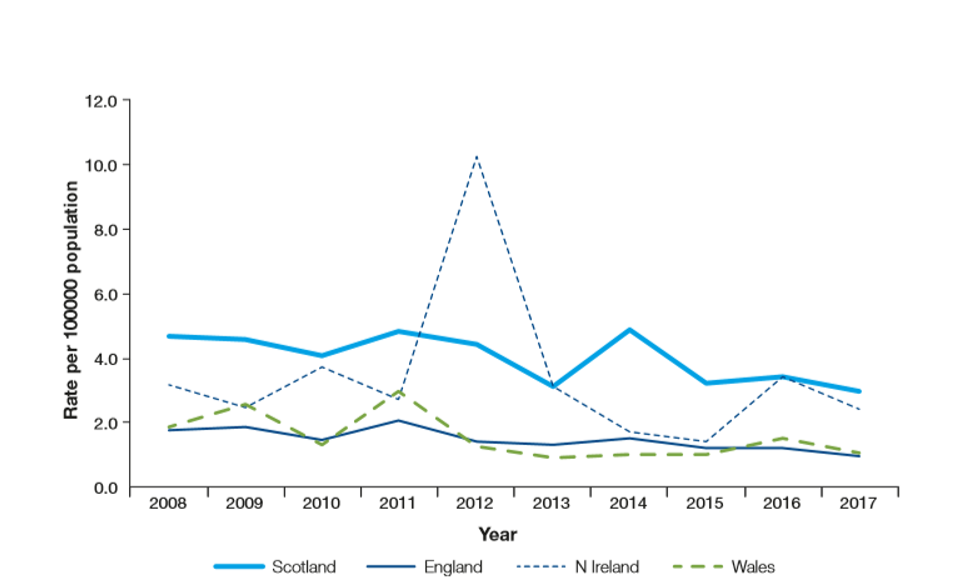
Scientists found that Scottish cattle have more E. coli O157 phage type (PT) 21/28, which is associated with super-shedding in cattle. Super-shedding is the passing of large volumes of the bacteria in feces. The report suggests local exposure to that particular subtype could be a factor for the rates of human infection in Scotland being about three times higher than in England and Wales.
From 1998 to 2012, Health Protection Scotland (HPS) reported a mean of 224 (205-243) culture positive cases of E. coli O157 annually. Of the 200-plus cases per year in Scotland, more than 40 percent required hospitalization and almost 10 percent developed severe renal complications.
Findings come from a four year research project involving Food Standards Scotland (FSS), the Food Standards Agency (FSA) and the United States Department of Agriculture’s Agricultural Research Service.
Research shows the overall prevalence of E. coli O157 in cattle is similar across Great Britain and has remained relatively consistent in Scotland for the last decade.
The consortium included the Roslin Institute, University of Edinburgh, Moredun Research Institute, Scotland’s Rural College, University of Glasgow, Public Health England, the Scottish E. coli O157/STEC Reference Laboratory (SERL), HPS and NHS Lothian.
Researchers used Whole Genome Sequencing (WGS) to tell which subtypes of E. coli caused an outbreak. For example, data from WGS helped to understand whether a human infection is likely down to local farm animals or by a strain present in imported food or after travel abroad. The team also combined WGS data with machine learning to predict which subtypes of E. coli O157 pose the greatest threat to human health.
Jacqui McElhiney, FSS’s head of food protection science and surveillance, said the report has produced new findings that will contribute to reducing the risks of E. coli.
“Scotland has historically had the highest levels of E. coli O157 infection in the UK and, despite our best efforts, the number of people affected has remained stubbornly stable. This research has shed some light on the possible reasons for this, and it’s really encouraging to see the progress that has been made in developing a potential vaccine for controlling it,” she said.
Surveys of the prevalence of E. coli O157 in fecal pats across 110 farms in Scotland and 160 in England and Wales were completed between Sept. 2014 and Nov. 2015. It was detected in at least one sample from 26 of the Scottish farms and from 34 of the farms in England and Wales.
In Scotland, PT21/28 was the dominant PT in cattle and 65 percent of positive farms (17 of 26) had cattle shedding it. For England and Wales PT21/28 was only found on three farms in the North East, Wales and West Midlands. The diversity of O157 PTs was much higher in cattle in England and Wales compared with Scotland.
In Scotland, season and some management/demographic characteristics were associated with farm O157 status, including moving breeding females onto the farm and purchase of livestock other than cattle in the year prior to sampling.
Researchers established that Shiga toxin (Stx) subtype 2a is important for transmission of E. coli O157 between cattle as it enabled bystander animals in a group to become colonized following introduction of an animal excreting the pathogen.
Different animal-targeted interventions to reduce excretion of E. coli O157 from cattle have been investigated including drinking water treatments, dietary, probiotics or feed additives, farm biosecurity, use of bacteriophages and vaccines. A systematic review found probiotics and vaccines (neither of which are commercially available in any country) were the most promising interventions.
Researchers also trialled a vaccine, developed to limit E. coli O157 excretion from and transmission between cattle. Results indicated it may be effective in reducing human exposure and infection. However, before a vaccine can be made available, further work is needed to assess if it is practical and works in field situations.
Modelling by Glasgow University found the vaccine would be an effective public health intervention. Attempts are underway for funding to support a feedlot trial of the vaccine formulation in the U.S.
Professor David Gally, from the Roslin Institute, said the study helped to understand how common E. coli O157 is across farms in Great Britain.
“We have found that what makes the strains toxic in humans also facilitates their colonisation of cattle. We have made advances in development of a vaccine for use in cattle that now needs assessment in large scale field trials. Modelling indicates that such an intervention would have significant public health benefit,” he said.
(To sign up for a free subscription to Food Safety News,
click here.)







