More than 1,500 confirmed Shiga toxin-producing E. coli (STEC) infections were reported in England and Wales in 2018 and five people died, according to Public Health England data.
A total of 1,553 confirmed cases included 607 laboratory-confirmed cases of STEC serogroup O157 and 612 infections where a non-O157 serogroup was isolated. In 2017, 948 confirmed cases of STEC were reported.
For 334 cases, samples tested positive by Polymerase Chain Reaction (PCR) for Shiga toxin (stx) genes, but STEC was not cultured with more than 300 of these in England.
Four STEC outbreaks caused by O157 affecting 55 people were investigated in 2018. It was not possible to find the vehicle and/or source of infection for the two largest and national outbreaks were a foodborne source was suspected. In one of these, 26 people were ill with 10 needing hospital treatment. In the other, 17 people were sick and four were hospitalized. The other two smaller outbreaks involved a petting farm and an outdoor event.
Data for STEC O157
The number of STEC O157 cases in England increased in 2018, but remained below pre-2015 levels. A reason for the decline in recent years is unclear, according to PHE.
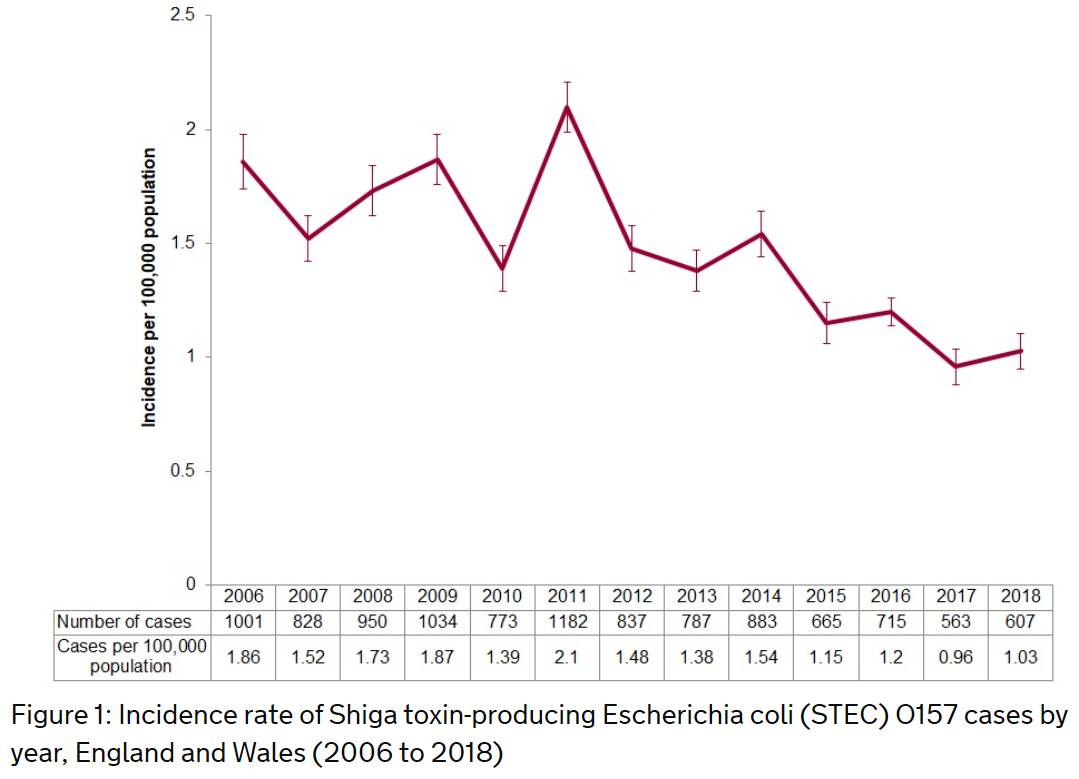
The STEC O157 figure of 607 has gone up from the 563 infections in 2017 but is below the 715 in 2016. As in previous years, STEC O157 had a peak of infection in the summer months.
Highest incidence was in children under 5 years of age. Nearly one-third of confirmed STEC O157 cases were hospitalized and 2 percent developed hemolytic uremic syndrome (HUS), a life-threatening condition predominantly affecting the kidneys. One death was reported.
Of 584 confirmed STEC O157 cases in England, 340 were female. Children aged 1 to 4 years had the highest incidence of infection. Overall, females had a higher incidence across all age groups, except for those 80 and older.
Based on data from 574 questionnaires, symptoms were reported for 549 cases; 93 percent had diarrhea, including 54 percent with bloody diarrhea. Other symptoms included abdominal pain, vomiting, nausea, and fever. Hospitalization was required in 28 percent of cases with duration ranging from 1 to 16 days.
HUS happened in 14 confirmed STEC O157 cases and most were under 5 years of age. HUS occurred in all three probable cases. Two were female aged from 8 to 14 years old.
A total of 146 cases were travel-associated and 33 spent the entire incubation period abroad. Top travel destinations included Turkey, Egypt, and Spain.
As with past years, phage type (PT) 8 and 21/28 were the main STEC O157 phage types, with a combined proportion of 51 percent. These were followed by PT 54, PT 32 and PT 14.
Rise in non-O157
Data comes from the National Enhanced Surveillance System for STEC infection in England (NESSS). Lab data for cases in Wales are from the PHE Gastro Data Warehouse (GDW).
Detection of non-O157 STEC infections continued to rise in 2018 to 612 and reflects the more widespread use of PCR in frontline labs to detect a broader range of serogroups, according to PHE.
The non-O157 figure of 612 in 2018 is much higher than the 385 reported in 2017.
In England, the most commonly reported non-O157 STEC serogroup was O26 with 17 percent of cases followed by O91, O146, O128ab and O117.
Seventy-five people were hospitalized and 24 developed HUS. Four deaths were reported among cases of non-O157 STEC.
Of the 567 non-O157 STEC cases in England, 73 different serotypes were confirmed. In Wales, for 45 cases 20 serotypes were recorded.
Questionnaires were received for 257 non-O157 STEC cases, and 46 STEC cases confirmed only by PCR. Of those symptomatic, 90 percent reported diarrhea, including bloody diarrhea. This was accompanied by abdominal pain, nausea, fever, and vomiting.
(To sign up for a free subscription to Food Safety News, click here.)








