The number of E. coli infections recorded in Scotland increased in 2018, according to a report on surveillance data from the country.
Cases of E. coli O157 decreased while non-O157 Shiga toxin-producing E. coli (STEC) increased. About a third of the infected people were admitted to hospitals for at least one night during their illness.
Of the 218 people for which information was available, 27 percent were considered to have acquired their infection outside the United Kingdom.
E. coli O157 decline
Rates of E. coli O157 infection in Scotland rose substantially in the mid-1990s and remain high compared to other countries within the U.K. and Europe.
Health Protection Scotland (HPS) reported the figures reflect normal variation expected from year to year but consistently high rates and the fact that a third of cases needed hospital treatment reinforces the need to apply the range of existing control measures found in food safety and other guidance.
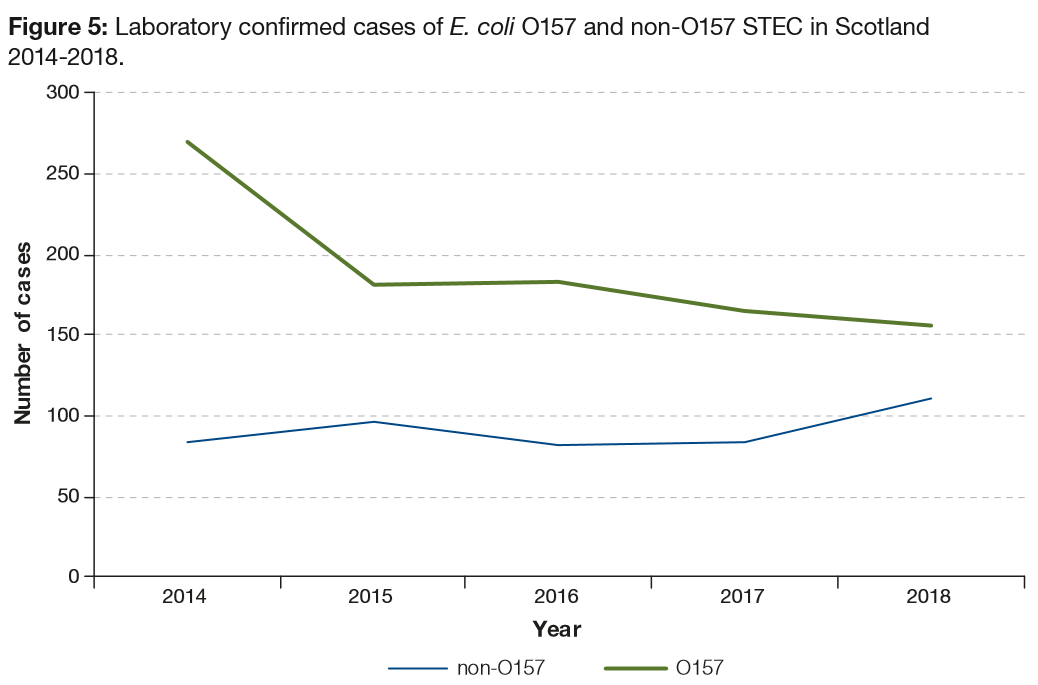
In 2018, 156 cases of confirmed E. coli O157 infections were reported to HPS, representing a slight decrease on the 165 the year before and 183 infections in 2016.
The age distribution of the 156 cases ranged from less than one to more than eighty years of age. More than half were female, 44 percent male. Children under 16 years of age accounted for 35 percent of cases and 10 percent of victims were older than 65 years. As seen in previous years, children younger than five had the highest rate of infection.
Incidence rates varied across Scotland, as they have done historically. As in most years, cases tend to peak in the summer months. Most infections were in the second and third quarters of the year, with 64 percent in this time period.
As in previous years, phage type (PT) 21/28 and PT8 remain the two most frequently reported. However, unlike previous years, PT8 was most commonly reported (33.3 percent), compared to 18.1 percent in 2017. This follows the declining trend in recent years in the proportion of PT21/28.
Non-O157 STEC increase
Diagnostic laboratories investigate all diarrheal feces for presence of E. coli O157 and refer isolates to the Scottish E. coli O157/STEC Reference Laboratory (SERL) for confirmation and further typing. STEC of serogroup O157 are the only ones for which routine standard tests are performed in diagnostic labs. Identification of non-O157 STEC requires submission of high risk fecal samples to SERL for investigation.
In 2018, there were 110 cases of non-O157 STEC reported to HPS compared to 83 cases in 2017 and 82 in 2016. Cases of non-O157 STEC accounted for 41 percent of all STEC reports.
Thirty different non-O157 STEC serogroups were identified, of which 19 were reported once only. STEC O26 was the most common serogroup and accounted for 34 culture confirmed cases. The two most commonly reported serogroups, O26 and O145, made up 52 percent of all culture confirmed non-O157 STEC cases.
During 2018, six outbreaks of E. coli O157 and STEC were reported; three of E. coli O157, two of E. coli O145 and one of E. coli O26. This is comparable to the number of outbreaks from 2013 to 2017, where there was an average of five and a range of three to nine incidents per year.
In five outbreaks last year, the main mode of transmission was considered to be foodborne and in the sixth it was a combination of foodborne and person to person.
(To sign up for a free subscription to Food Safety News, click here.)









