Opinion
“Tropical parasites in our food? No way!” most Americans think.
It’s time to think again.
In May Hawaii’s Department of Health announced three more cases of rat lungworm in recent visitors. Already endemic in Hawaii, Asia, Australia, Brazil and the Caribbean, the exotic foodborne menace is also emerging in Florida and other southeastern states.
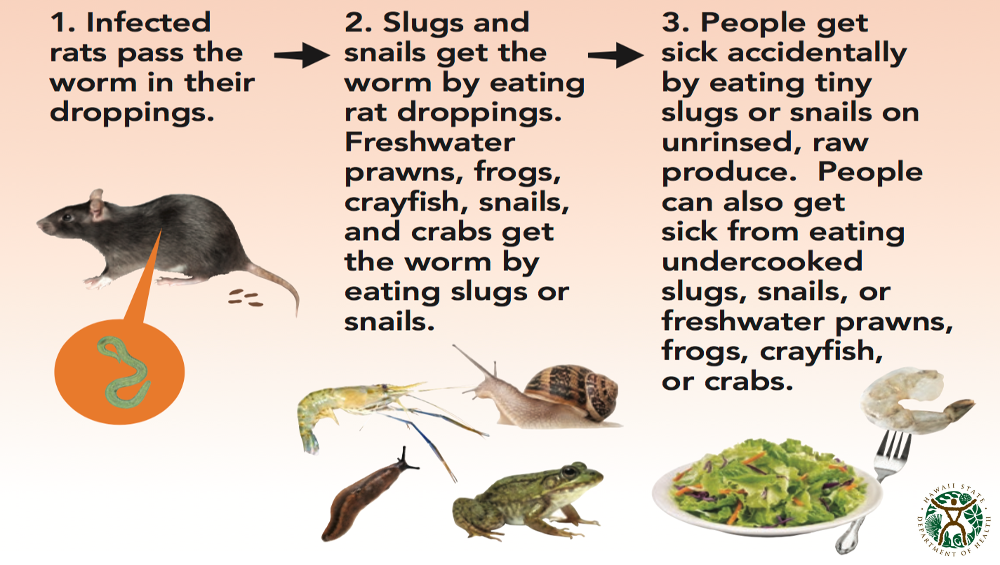
Rat lungworm survives using clever, earthy tactics. Adult worms live in rats—snails and slugs get infected by eating rat droppings—rats get infected by eating parasite-laden snails and slugs. Humans are “dead-end hosts,” meaning we can’t transmit the disease to others. But we can still fall gravely ill when larvae migrate, grow and die in our brains.
Last year, ten people officially contracted rat lungworm in Hawaii, presumably from eating locally-grown greens harboring mollusks. But human cases are underreported, according to the state’s Department of Health. Consider the risk in fauna. In Hawaii, up to 70 percent of a newly-invasive semi-slug carry rat lungworm larvae, while a 2017 Florida study found the parasite in one in five rats and one in 50 snails. In Florida, it has killed or sickened zoo animals; in neighboring states, it has also sickened a handful of humans.
What if plants grown in Hawaii or the Southeast spread infected mollusks to new locales? If tiny, larval-laden snails enter the Salinas Valley—especially if temperatures and rainfall continue to climb—could California’s leafy greens someday spawn cases? We believe the answer is yes.
The risk to tourists is equally worrisome. More than 9 million visit Hawaii every year and visitors have developed the disease. Returning travelers face many diagnostic obstacles, including the lack of definitive blood tests.
In the 1980s, one of us saw toddlers in Taiwan initially diagnosed with bacterial meningitis before unusual cells in their spinal fluid pointed to rat lungworm. Thirty years later, the situation hasn’t changed. Unless a doctor thinks of it, then performs a spinal tap, requests special tests and prescribes the right medications, patients can suffer dire harm.
More lessons can be gleaned from a landmark outbreak. In 1999, 23 medical students traveled to Jamaica on spring-break and shared a final celebratory feast. Weeks later, eleven of the twelve who ate Caesar salad tested positive for rat lungworm at the CDC. Three sufferers were well enough to remain outpatients, while a fellow student was hospitalized for weeks and—despite intravenous steroids—required a dozen spinal taps to relieve sky-high pressure in her brain.
Saddest of all is the story of Sam Ballard from Australia. In 2010, while in Sydney, the 19-year old ate a slug on a dare, thus contracting rat lungworm. After awakening from a coma, Ballard was fully paralyzed, and in 2018, he died. Hawaii has witnessed similar tragedies.

What can be done?
In Hawaii, especially near Hilo, a non-native semi-slug with high larval loads likely accounts for worsening infections. This small species with a toenail-sized shell on its back enters gardens, houses and water tanks. Controlling the semi-slug and other intermediate hosts is an uphill but necessary battle.
Physicians on the mainland still lack knowledge about rat lungworm disease. Education is needed, as are better diagnostic tests.
Education is also needed for visitors to Hawaii, Florida and other places where the parasite is present. Sensible advice? Eat only local produce that has been thoroughly washed. Don’t throw fresh leafy greens into a blender for a Kermit-colored smoothie. Don’t drink from a hose where a snail or slug might hide. Don’t let children play with snails!
Finally, what rat lungworm teaches is the dynamic ecology of foodborne parasites and one more basic truth. Parasites are not just “over there” — but here.
Cyclospora, which causes diarrhea, is another example. Until last year, foodborne outbreaks in the U.S. were solely linked to produce imported from Central and South America. But in 2018, a salad mix from California caused more than 500 cases in people who ate at fast-food restaurants in 15 states and New York City. Not only was Cyclospora found in unopened bags of the salad mix, it was also detected for the first time in romaine grown on California farms.
Human infections due to foodborne parasites are preventable. We should all stay vigilant and informed, not just about rat lungworm, but the next emerging threat. And the next. After all, from a parasite’s point of view, it’s all about surviving and thriving, which is what the rat lungworm has done for millennia.
About the author: Claire Panosian Dunavan is an infectious diseases specialist at UCLA and a past-president of the American Society of Tropical Medicine and Hygiene. Stephen Ostroff most recently served as FDA’s deputy commissioner for food and veterinary medicine.
Publication note: This column originally appeared in The Hill and is republished here with permission.
(To sign up for a free subscription to Food Safety News, click here.)








