
Healthcare providers, caregivers, researchers and suppliers gathered at the 43rd annual meeting of the Association for Professionals in Infection Control & Epidemiology (APIC) in Charlotte, NC, June 11-13. The theme was “Inspiring Innovation in Infection Prevention” and attendees discussed how evidenced-based research can resolve the recurring riddle of risk versus budgets for both foodservice and skilled nursing facilities. Motivating innovations in foodborne outbreak prevention was an unstated goal but an important byproduct of the meeting. All hospitals and nursing homes prepare and serve food for the most vulnerable populations. The CDC attributes Healthcare Associated Infections (HAIs) as the cause of death for 99,000 hospital patients annually and 380,000 in nursing homes. The year-to-date reference point is carried to the state level at this website: http://handwashingforlifehealthcare.org/healthcare-deaths Personnel from the Handwashing For Life Institute were unsuccessful in attempts at APIC to locate peer reviewed estimates on the percentage of these deaths due to the food preparation, delivery and feeding of the patients and residents.

Busting myths about gloves, hot water and hand sanitizers Deep dives into measuring new factors in infection transmission exposed flaws in food handling and overall patient protection systems. Sessions challenged such basics as “To Glove or Not To Glove” and busted many a myth. Deborah Burdsall presented findings she has discovered in her doctoral work on this topic at the University of Iowa. Research illustrates that we in the USA are overusing gloves but under-changing them when a clean, gloved-hand is most essential in protecting the at-risk population. Glove use and misuse is deeply psychological and thus very difficult to align behaviors with the science and the guidelines of the FDA or CDC. Caregivers at the annual meeting attended sessions starting as early as 5:30 a.m. where they were challenged to think about the advantages of washing hands with cool water after years of guidance under the Model Food Code to use hot water. Evidenced-based research shattered the myth that alcohol hand sanitizers are drying to the hands, causing Irritant Contact Dermatitis (ICD). Poorly formulated soaps, particularly those which are not easily rinsed, are the culprits. Formulation matters.
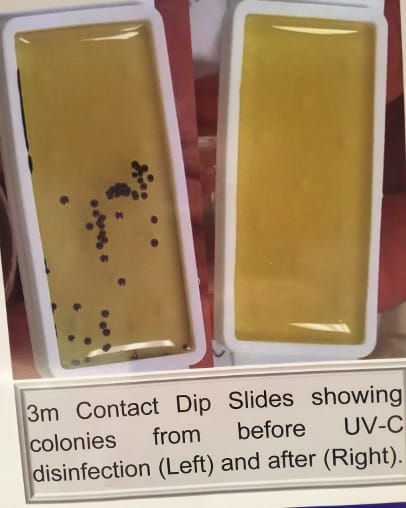
Sometimes more money means fewer infections, which means money saved High-tech challenges were also on the menu. Much of the meeting content recognized that the majority of unresolved issues in patient safety required behavior changes and changes of culture, from the boardroom to the caregiver. Most all require significant investment but offer greater savings in lower infection rates. Two specific technologies were well represented and integrated from the show floor through to educational sessions and in an array of poster presentations. Electronic Hand Hygiene Monitoring (EHHM) and ultraviolet (UV-C) surface disinfection are both problem-solving advancements but both require a strong business case to initiate. HAI costs are well documented and their reduction often has a payback within the first year. But getting started is still a hard sell in some corporate settings. The growth of ultraviolet in killing resistant pathogens was summarized by Gunner Lyslo, founder and CEO at Surfacide LLC. He said UV-C is a good example of applied innovation. It is an evidence-based technology that not only is effective in reducing pathogens in patient rooms but more importantly is improving patient outcomes. Documented performance directly connected to lowering HAIs is driving the current surge of usage. The Affordable Care Act incentivizes higher performance with its scale of reimbursements from the punitive to the positive rewards for outstanding outcomes. This innovation is quickly becoming the standard, Lyslo said. According to APIC 2016 keynote speaker Dr. William Rutula from University of North Carolina Health System, “If you don’t have these systems, you should have them in your capital budget.”

Overwhelming innovation, underwhelming implementation Innovation can drive behavior change but effective and enduring solutions start with leadership in realistic risk assessment and the early engagement and empowerment of the program creators, implementers and maintainers. Yes, APIC sees the R in ROI as “return” but also as lives saved. The I is for “investment,” but they are looking to “innovation” to accelerate patient safety initiatives. ROII, or I squared, Return On Investments in Innovation, is a call for all to learn business speak when trying to improve care. Business drives the care. Let’s all learn the language. Neither infection prevention nor quality assurance arguments are effective funding factors by themselves. They both require evidence converted to revenue. All foodservice and care providers in general are risky businesses, getting riskier as the government amps up its array of penalties as a more efficient way to “motivate” compliance rather than adding more facility auditors. Scientific advancements, such as Whole Genome Sequencing, contribute to the rising risk as tracking the infection back to its source of infection is getting faster and more accurate. Progress in risk modeling, including quantitative risk assessment, is making it easier to build better business cases to invest in enhanced patient care and foodservice innovations. University of Arizona’s Kelly Reynolds presented one such powerful advancement: “Once we find the pathogens, it is important to quantify the risk and identify the effective interventions. Our team is continuously enhancing these decision support models.” Make your business case:
- Measure your risk and opportunity.
- Set your standards.
- Optimize processes.
- Train to the standards.
- Motivate with evidence-based outcomes.
(To sign up for a free subscription to Food Safety News, click here.)







