ROSEMONT, IL — Roslyn Stone, who manages health incidents for many of the nation’s largest restaurants and foodservice chains as the chief operating officer for Zero Hour Health, clearly has Dr. Monique Foster, who is epidemiology lead for hepatitis A at the Division of Viral Hepatitis at the Centers for Disease Control and Prevention (CDC0 in Atlanta, on her speed dial.
At the CDC, Foster is fighting the widespread person-to-person outbreaks of hepatitis A that have plagued specific U.S. cities and states since first identified in 2016. Across 34 states, hepatitis A outbreaks from 2016 to Oct. 16, 2020, have involved 35,578 confirmed patients with 21,744 ,or 61, percent requiring hospitalization and 336 deaths. Speaking virtually from the Food Safety Summit, Foster said that from 2014 to 2018, the Hep A outbreaks occurring across the country represented an 850 percent increase in Hep A cases.
Stone and Foster jointly put on a live session for the Summit on how the response to the Hep A outbreaks has helped combat COVID-19 and might be bringing the Hep A outbreaks to a close. Before COVID-19 arrived, Hep A led the restaurant health incidents that required Stone’s response. Others included norovirus, measles, and mumps.
While Hep A can be spread through foodborne transmission by ingestion of contaminated food and drink, that’s been rare. What’s been happening lately, according to Foster is the person-to-person transmission with an infected person and recently that’s meant someone from a specific at-risk group — drug users, the homeless, and men who have sex with men — topping the list.
The hepatitis A Virus (HAV) replicates in the liver and is excreted in bile. Foster says it is an “acute illness” known for causing fever, jaundice, myalgia, anorexia, malaise, and diarrhea. It has an average incubation period of 28 days with a range of 15 to 50 days. Infections peak from 10-14 days prior to showing symptoms to 7-10 days after the onset of symptoms. Foster says the lengthy times make Hep A difficult to investigate.
She calls the Hep A virus “small but mighty” due to it remaining stable outside the body for months, and the ability to withstand temperature variances — including freezing — and other characteristics.
Hep A is associated with international travelers in the U.S. because the number of other incidents has historically been low.
Foster says that while “person-to-person” contact is responsible for the vast majority of the current outbreaks and involves people from the impacted groups, there is a “bias” in public awareness. That’s because reporting about outbreaks largely focuses on when restaurant customers might have been exposed to an infected restaurant worker. In such instances, CDC favors doing an evaluation to determine how likely it was that the infected restaurant or foodservice worker would have infected a customer or co-worker while on the job.
The agency does not favor public notification in all instances, only when time remains to make vaccinating restaurant employees or customers worthwhile.
“Secondary transmissions do occur,” says Foster. But she reports that secondary infections from food handlers are low — less than 1 percent of all the cases. It means that preemptively vaccinating all food handlers would be ineffective at mitigating the current risk of the person-to-person outbreaks.
Foster says local health departments should assess risk on a case-by-case basis and target vaccinations at high-risk populations. Most of the infected food handlers identified by CDC surveys are in fact high-risk group members who just happen to be employed in the restaurant industry.
Foster encourages the prevention of foodborne transmission of the hepatitis A virus by property handwashing; eliminating bare hand contact with food; open discussion by managers and employees about symptoms and diagnoses, exclude or restrict employees with symptoms of Hep A infections; and awareness of state-specific exclusion policies.
Stone says learning to respond correctly to Hep A incidents has helped with the response to COVID-19. She says the novel virus is surging in many states, large numbers of restaurant employees are “excluded” for exposure having the illness, and changing state and local requirements remain a challenge. The first of the seasonal flu cases began occurring two weeks ago. Mask and glove use is now standard across the country, with a focus on handwashing and temperature checks.
“We don’t know if this is the second surge or the third surge,” she says. But every day a dozen states see rising COVID numbers.
Stone says some state and local health departments are “going public” with just one COVID-19 case. Depending on the jurisdiction, that can mean 10 to 14 days “exclusions” preventing the employee from working, the need to clean and sanitize the restaurant or facility, and the beginning of “contact” tracing to find those who spent 15 minutes within six feet of the sick person, or even less time depending on the state.
The restaurant industry, she says, has refocused on wellness checks, hand washing, and making sure people who are sick do not come to work.
Stone told the virtual conference attendees that much was learned from Hep A., including the need for wellness checks, keeping sick employees at home, hand washing and how to respond to an incident. Work schedules are Hep A’s version of contact tracing and the incidents taught the need for keeping vaccinations histories.
Stone said the restaurant industry went from four Hep A incidents a year to four per week with the current outbreaks.
The frequency of the Hep A events has brought change to the restaurant industry. Managers know they can no longer encourage an ill employee to just stay through the lunch rush. “We’ve really learned from Hep A that we cannot let that happen,” Stone said.
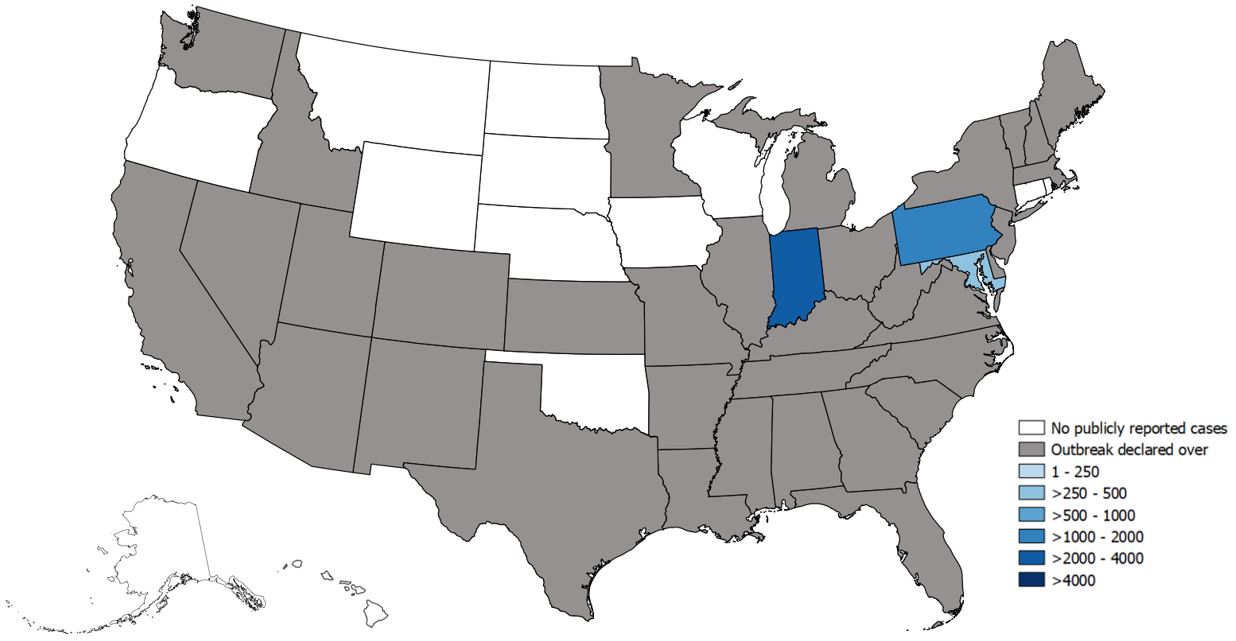
Progress is being made with the Hep A outbreaks. Five Southwestern states have declared an end to their outbreaks, and at least a dozen more haven’t experienced any significant amount of cases. The CDC’s latest status report continues below.
State-Reported Hepatitis A Outbreak Cases as of Oct. 16, 2020
| State | Case Total | Hospitalizations n (%) | Deaths | Outbreak Start Date | Data Current Through |
| Total | 35578 | 21744 (61%) | 336 | ||
| States with an ongoing outbreak | |||||
| Alabama | 838 | 565 (67%) | NR | 9/1/2018 | 8/31/2020 |
| Arkansas | 482 | 256 (53%) | 3 | 2/7/2018 | 3/6/2020 |
| Colorado | 405 | 288 (71%) | 2 | 10/1/2018 | 9/30/2020 |
| Delaware | 38 | 22 (58%) | 1 | 8/1/2019 | 9/23/2020 |
| Florida | 4592 | 3221 (70%) | 70 | 1/1/2018 | 8/31/2020 |
| Georgia | 1353 | 874 (65%) | 8 | 6/1/2018 | 10/10/2020 |
| Idaho | 74 | 37 (50%) | 0 | 1/1/2019 | 8/13/2020 |
| Illinois | 195 | 132 (68%) | 1 | 9/1/2018 | 6/23/2020 |
| Indiana | 2393 | 1335 (56%) | 4 | 11/1/2017 | 7/3/2020 |
| Kansas | 108 | 95 (88%) | 0 | 1/12/2020 | 10/16/2020 |
| Kentucky | 5001 | 2411 (48%) | 62 | 8/1/2017 | 2/8/2020 |
| Louisiana | 1303 | 769 (59%) | 4 | 1/1/2018 | 10/16/2020 |
| Michigan | 920 | 738 (80%) | 30 | 8/1/2016 | 2/5/2020 |
| Minnesota | 123 | 85 (69%) | 1 | 12/16/2018 | 10/9/2020 |
| Mississippi | 187 | 129 (69%) | 0 | 4/1/2019 | 2/26/2020 |
| Missouri | 697 | 403 (58%) | 2 | 9/1/2017 | 3/14/2020 |
| New Hampshire | 319 | 198 (62%) | 2 | 11/1/2018 | 2/11/2020 |
| New Jersey | 623 | 408 (65%) | 7 | 12/1/2018 | 2/22/2020 |
| New York (excluding New York City) | 391 | 262 (67%) | 0 | 6/1/2019 | 10/10/2020 |
| North Carolina | 346 | 223 (64%) | 2 | 1/1/2018 | 10/7/2020 |
| Ohio | 3689 | 2294 (62%) | 16 | 1/1/2018 | 10/12/2020 |
| Pennsylvania | 863 | 666 (77%) | 14 | 1/1/2018 | 10/10/2020 |
| South Carolina | 1660 | 875 (53%) | 5 | 11/1/2018 | 10/9/2020 |
| Tennessee | 3036 | 1839 (61%) | 28 | 12/1/2017 | 5/8/2020 |
| Vermont | 14 | 6 (43%) | 0 | 1/1/2019 | 7/11/2020 |
| Virginia | 435 | 272 (63%) | 2 | 1/1/2019 | 10/9/2020 |
| Washington | 366 | 212 (58%) | 5 | 4/1/2019 | 6/22/2020 |
| West Virginia | 2702 | 1366 (51%) | 23 | 3/19/2018 | 2/28/2020 |
| States with a declared end to their outbreak | |||||
| Arizona | 598 | 484 (81%) | 8 | 11/1/2018 | 4/16/2020 |
| California | 708 | 464 (66%) | 21 | 11/1/2016 | 4/11/2018 |
| Massachusetts | 563 | 442 (79%) | 9 | 4/1/2018 | 5/29/2020 |
| Nevada | 107 | 94 (88%) | 1 | 11/1/2018 | 6/18/2020 |
| New Mexico | 168 | 127 (76%) | 2 | 11/8/2018 | 6/10/2020 |
| Utah | 281 | 152 (54%) | 3 | 5/8/2017 | 2/12/2019 |
NR: not publicly reported
- “Outbreak-associated” status is currently determined at the state level in accordance with each state’s respective outbreak case definition.
- Outbreak-related hepatitis A deaths are defined at the state level in accordance with each state’s respective hepatitis A-related death definition. Some states are reviewing death certificates on a regular basis to actively find hepatitis A-related deaths, while other states are utilizing passive surveillance.
- Outbreak start date is defined at the state level and may represent the earliest onset date of an outbreak case (AR, AZ, KS, UT), the left censor date for which cases are considered part of the outbreak based on the state outbreak case definition (AL, CA, CO, DE, FL, GA, ID, IL, IN, KY, LA, MA, MI, MN, MO, MS, NV, NH, NJ, NC, OH, PA, SC, TN, VA, WA), or when a state declared a hepatitis A outbreak (NM, WV).
(To sign up for a free subscription to Food Safety News, click here.)









