University of Arizona researchers have created a portable method for detecting low levels of norovirus.
The analysis is done automatically by a smartphone app when a sample of water is loaded onto the chip.
Detecting very small amounts of norovirus in water or food samples typically involves a polymerase chain reaction (PCR)-based method, which takes several hours and is done in a lab by trained personnel.
Noroviruses are the top cause of foodborne illness. A person usually develops symptoms 12 to 48 hours after being exposed to the virus. Most people get better within one to three days. During 2009 to 2015, the Foodborne Disease Outbreak Surveillance System (FDOSS) received reports of 1,130 norovirus outbreaks and 27,623 outbreak-associated illnesses.
“It only takes a very small number of norovirus particles to cause an infection in humans, so we need a really sensitive detection method. Also, scientists aren’t able to culture norovirus in the lab, and available antibodies to the pathogen aren’t very strong,” said Jeong-Yeol Yoon, who led the team, which included Soo Chung and Kelly A. Reynolds.
They published their results in ACS Omega, a journal of the American Chemical Society, and Yoon presented the research at the ACS Fall 2019 National Meeting & Exposition in San Diego.
From light scattering to fluorescence
In previous work, the team developed a smartphone-based device that could detect low levels of norovirus by measuring the light scattered from virus-bound polystyrene beads in a paper microfluidic chip.
Paper’s porousness and opacity can cause background scattering that interferes with imaging and makes it difficult to detect very small concentrations of a virus. The new approach involves counting fluorescent beads instead of measuring light intensity.
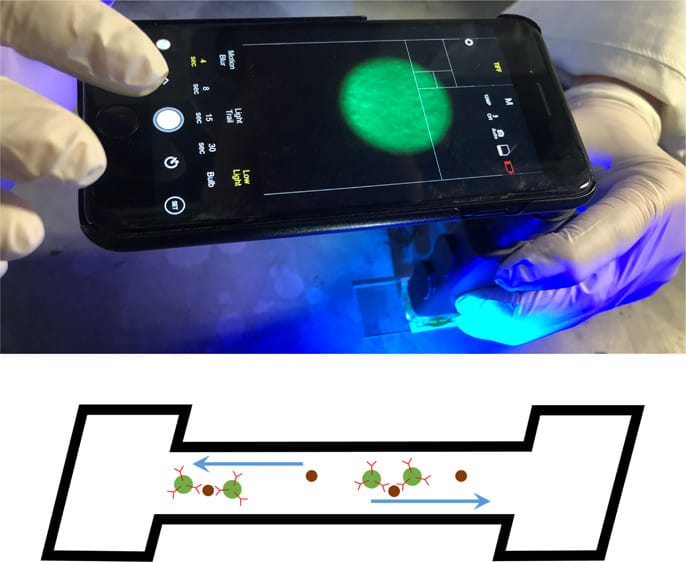
Researchers converted a smartphone into a fluorescence microscope by attaching a commercially available light microscope accessory, a separate light source, and two band-pass filters. To a channel of their paper microfluidic chip, they added a water sample containing norovirus.
The team added a suspension of fluorescent beads with antibodies against norovirus attached. The capillary action of the paper caused the two liquids to flow and mix. Each individual norovirus particle bound to multiple fluorescent beads via their attached antibodies, causing the beads to aggregate and produce a much larger size of the fluorescent image.
“Norovirus particles are too small to be imaged by a smartphone microscope, and so are antibodies. But when you have two or three or more of these beads joined together, that indicates that the norovirus is there, causing the beads to aggregate,” said Yoon.
They took photos of the chip with their smartphone-based fluorescence microscope, and an app calculated norovirus concentrations from the pixel count of the images. The most expensive part of the whole device is the smartphone microscope which costs less than $50.
Early diagnosis in patients
The lowest detection limit was about 5 or 6 norovirus particles per sample. As few as 10 virus particles can cause illness, so the method is sensitive enough for practical applications.
Yoon and colleagues made the system more compact by enclosing the fluorescent microscope, light source and optical filters in a 3D-printed case. They also developed a cloud-computing app to analyze the large images and send results to the smartphone. Finally, they found a way to concentrate samples within the paper chip to analyze larger sample volumes.
The device could detect small amounts of norovirus in purified water and reclaimed wastewater but had problems with tap water with scientists suspecting chlorine was affecting the assay.
Researchers are now working on using the smartphone-based device for diagnosing norovirus infections in patients at an earlier stage than is currently possible by analyzing fecal samples.
Early detection might help stop the spread of disease in isolated, crowded situations like cruise ships.
“When norovirus reaches levels detectable by other methods, the person is already seriously ill. But if we can detect the virus earlier, they can receive medical care sooner,” said Yoon.
The National Science Foundation Water and Environmental Technology Center at the University of Arizona and Tucson Water provided funding for the research.
(To sign up for a free subscription to Food Safety News, click here.)









