There has been a dramatic increase in the number of hepatitis E cases in France since 2010, according to researchers.
The rise can be attributed to the availability of hepatitis E virus (HEV) diagnostic tests and a better understanding of infection causing an increase in the number of people being tested and the incidence of autochthonous cases.
Pork, the main reservoir of HEV in France, can be the origin of food transmission, especially products made from raw liver. Research has shown swine are the main reservoir because of a high prevalence of HEV infection on pig farms. Prevention is based on informing consumers about the need to thoroughly cook such products.
In France, hepatitis E surveillance has been done by the National Reference Center (CNR) for enteric-transmitted hepatitis viruses (hepatitis A and E) since 2002.
The researchers’ objective was to describe HEV infection data sources and epidemiological results in France from 2002 to 2016. Two periods were differentiated for data analysis – 2002 through 2011 and 2012 through 2016 because of changes in the CNR and availability of more sensitive HEV tests.
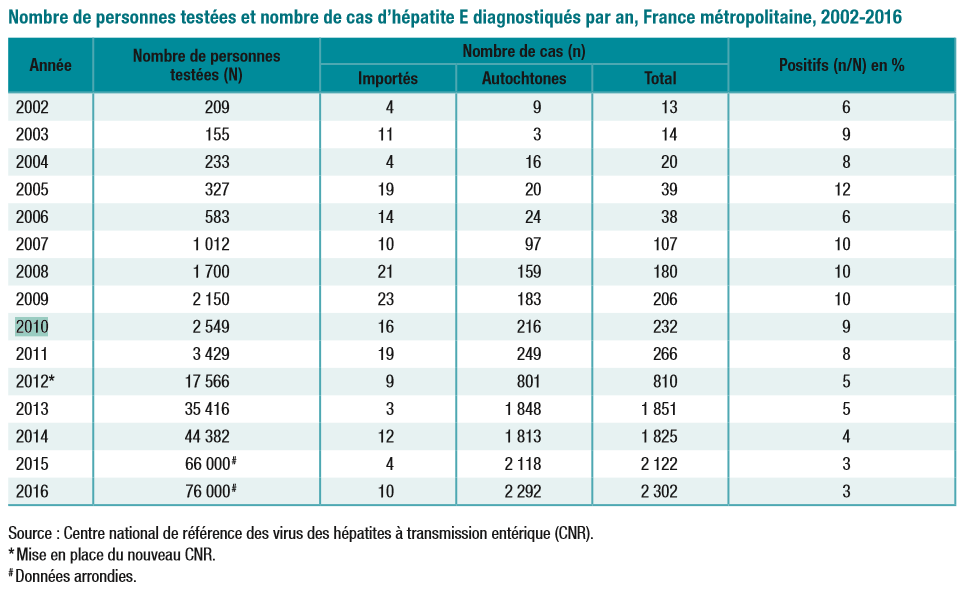
In this period, the number of people for whom samples were sent for a diagnosis of hepatitis E increased dramatically, 209 vs. 76,000. An increased number of diagnosed cases was also noted, primarily for autochthonous cases 9 vs. 2,292. The number of imported cases has stayed at a stable level. Since 2007, more than 90 percent of autochthonous strains, so-called native strains, were genotype 3.
The number of people hospitalized for hepatitis E increased from 57 to 653 with higher annual incidence rates in southern regions. The suspected source of contamination for clustered cases was most often consumption of raw pork liver sausages.
Autochthonous cases have not changed much since 2002 in terms of age and sex, with mostly men aged over 50 years impacted.
In the early 2000s, most cases of hepatitis E diagnosed in industrialized countries were among people who had traveled to a country where access to drinking water and sanitation was poorly controlled. Then autochthonous transmission was suspected in patients with no travel history which suggested sources other than water. The most frequently documented autochthonous transmission was food, by consumption of contaminated products from HEV reservoir animals such as pork, wild boar or deer.
In 2002, diagnosed domestic hepatitis E cases were low and knowledge of epidemiology was limited. From 2010 the availability of effective serological and molecular diagnostic tests and increased use of commercial tests resulted in an increase in the number of people tested with domestic cases far exceeding imported ones.
A French study published in 2011 showed that HEV circulates in 65 percent of pig farms and the prevalence of HEV-RNA in pig livers taken from the slaughterhouse, thus entering the food chain, was 4 percent.
Hepatitis E is not a notifiable disease in France, but measures are being taken to ensure trends and circulation of genotypes can be monitored.
Surveillance of hepatitis E by the CNR is based on the voluntary submissions from public and private laboratories of samples to confirm the diagnosis or for typing strains. The CNR also lists the annual activity of hospital labs practicing HEV diagnosis and two centralized private labs – Eurofins Biomnis and Cerba.
Since 2005, outbreaks of Hepatitis E have been investigated by Santé Publique France, regional health agencies and the CNR. These clusters were generally small with less than 10 cases.
Suspected sources of contamination have included lightly cooked or raw figatelli, a variety of sausage, homemade smoked ham, and water from a private well. A comparison of human and food strains was not possible in any of these investigations.
Mandatory labeling of raw pork liver products was introduced in 2009. Researchers said it was necessary to focus research on possible control measures on the circulation of hepatitis E virus in pig farms in industrialized countries.
Other sources of contamination are suspected such as consumption of shellfish, vegetables or fruits tainted by contact with dirty water. Contamination related to insufficient hand hygiene or through direct contact with live animals or their carcasses has also been suspected.
Cooking at 71 degrees C for 20 minutes inactivates Hepatitis E virus. The incubation period following exposure to the virus ranges from three to eight weeks. Diagnosis is usually based on the detection of specific IgM and IgG antibodies to the virus in the blood.
Typical symptoms include yellow discoloration of the skin and eyes, dark urine and pale stools abdominal pain and tenderness, nausea, vomiting and fever.
(To sign up for a free subscription to Food Safety News, click here.)









