The Centers for Disease Control and Prevention is reporting a multi-state outbreak of infections from the Cyclospora parasite that has sickened almost 100 people.
As of the agency’s most recent outbreak update, 97 people from 14 states have been confirmed infected by the microscopic parasite. Sixteen people have required hospitalization because their symptoms were so severe. Public health officials have not reported any deaths.
The total number of sick people has not yet been reported to the CDC because of the time it takes for testing and confirmation testing. Some individual case counts reported so far this year by state authorities include Colorado with 62 patients who ate at a single restaurant. Outbreak investigations are also underway in 15 other states.
Prior to the current update, the CDC first reported on the outbreak on May 25. The first date of onset of the infections was April 1. No specific food items have been identified as the source of the parasite.
Sick people range in age from 16 to 92 years, with a median age of 48. Seventy-one percent are female. The true number of patients is likely much higher than the confirmed number because many people do not seek medical attention. Antibiotics are required to kill the parasite.
Specific testing is required to confirm infection from the Cyclospora parasite because symptoms usually mimic other illnesses.
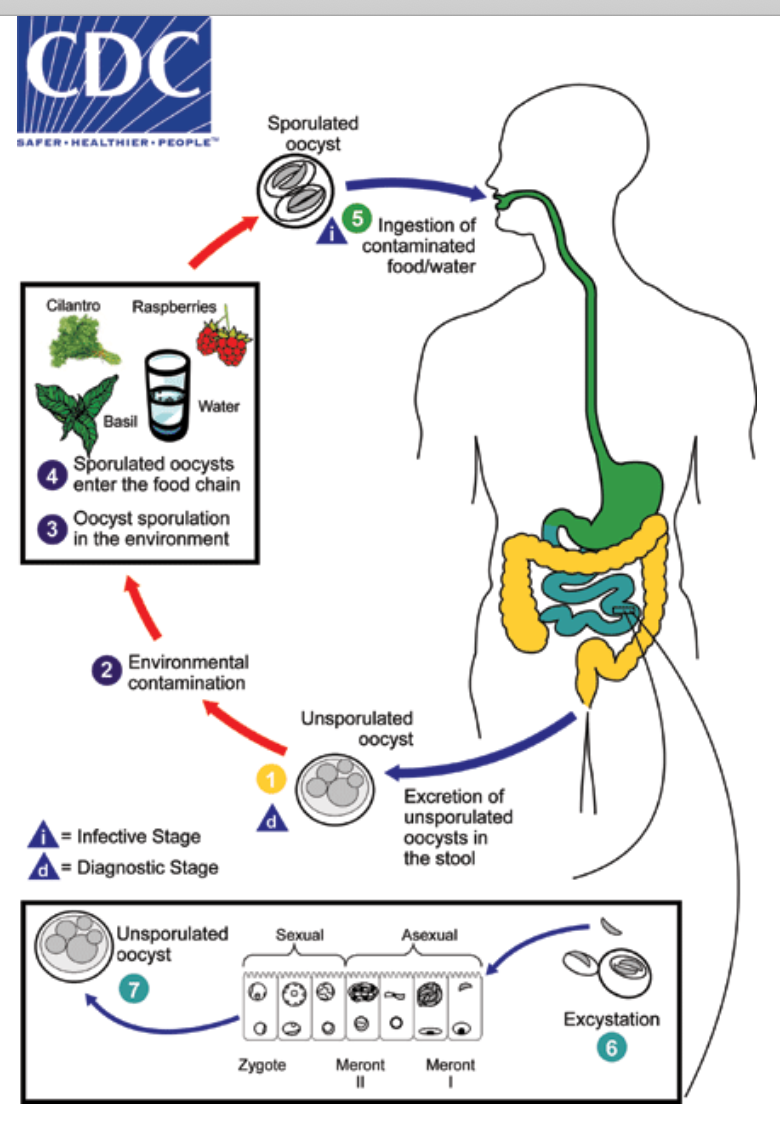
Symptoms usually start within two weeks after eating food contaminated with Cyclospora. People typically experience watery diarrhea. They may also experience loss of appetite, cramping, bloating, increased gas, nausea, and fatigue. Symptoms can persist for several weeks to a month or more. If untreated, symptoms may get better for a while and then return, and this pattern may repeat.
Identifying the particular food item or ingredient that caused an outbreak of cyclosporiasis can be very challenging. If fresh produce was served as a garnish or topping or if several types of produce were mixed together investigators often can’t determine what the source of the parasite was.
“Cyclosporiasis illnesses are reported year-round in the United States. However, during the spring and summer months there is often an increase in cyclosporiasis acquired in the United States,” according to the CDC outbreak notice.
“The exact timing and duration of these seasonal increases in cyclosporiasis can vary, but reports tend to increase starting in May. This year, cases were reported starting in April. It is too soon to tell if this timing indicates a change in the seasonality of cyclosporiasis in the United States.
“In previous years, the reported number of cases peaked between June and July, although cases can be reported as late as September. The number of infections or hospitalizations and the number of identified outbreaks linked to a common source also vary from season to season.”
Outbreaks of cyclosporiasis in the Untied States have been linked to various types of fresh produce, including basil, cilantro, mesclun lettuce, raspberries, and snow peas. However, many cases of cyclosporiasis cannot be directly linked to an outbreak.
Officials use questionnaires to interview sick people to determine what they ate in the 14-day period before getting sick. If a common food is found, CDC and partners work quickly to determine if the contaminated food is still available in stores or in peoples’ homes and issue advisories.
The table below provides information about 39 reported foodborne outbreaks of cyclosporiasis that occurred in the United States from 2000 to 2017. The total conformed case count was 1,730. No outbreaks were reported in 2003, 2007, or 2010. Many additional illnesses are likely but were not confirmed, according to the CDC.
Overall, a median of two outbreaks were reported per year, with a median of 19 confirmed patients cases per outbreak. Although the outbreaks occurred during 8 different months (December through July), the peak months were May, June, and July. As indicated in the table, a food vehicle of infection was identified (or suspected) for 17 of the 39 outbreaks.
| Table: Summary of U.S. foodborne outbreaks of cyclosporiasis, 2000–2017 | ||||
| Year(s)* | Month(s)* | Jurisdiction(s)* | No. of cases† | Food vehicle and source, if identified‡ |
| 2000 | May | Georgia | 19 | Raspberries and/or blackberries (suspected) |
| 2000 | June | Pennsylvania | 54 | Raspberries |
| 2001 | January–February | Florida | 39 | |
| 2001 | January | New York City | 3 | |
| 2001–02 | December–January | Vermont | 22 | Raspberries (likely) |
| 2002 | April–May | Massachusetts | 8 | |
| 2002 | June | New York | 14 | |
| 2004 | February | Texas | 38 | |
| 2004 | February | Illinois | 57 | Basil (likely) |
| 2004 | May | Tennessee | 12 | |
| 2004 | May–June | Pennsylvania | 96 | Snow peas from Guatemala ⁂ |
| 2005 | March–May | Florida | 582 ¶ | Basil from Peru |
| 2005 | May | South Carolina | 6 | |
| 2005 | April | Massachusetts | 58 | |
| 2005 | May | Massachusetts | 16 | |
| 2005 | June | Connecticut | 30 | Basil (suspected) |
| 2006 | June | Minnesota | 14 | |
| 2006 | June | New York | 20 | |
| 2006 | July | Georgia | 3 | |
| 2008 | March | Wisconsin | 4 | Sugar snap peas (likely) ⁂ |
| 2008 | July | California | 45 ¶ | Raspberries and/or blackberries (likely) |
| 2009 | June | District of Columbia | 34 | |
| 2011 | June | Florida | 12 | |
| 2011 | July | Georgia | 88** | |
| 2012 | June–July | Texas | 16 | |
| 2013†† | June | Iowa, Nebraska, and neighboring states | 162 | Bagged salad mix from Mexico |
| 2013†† | June–July | Texas | 38 | Cilantro from Mexico |
| 2013 | July | Wisconsin | 8 | Berry salad (suspected) |
| 2014 | June | Michigan | 14 | |
| 2014‡‡ | June–July | Texas | 26 | Cilantro from Mexico |
| 2014 | July | South Carolina | 13 | |
| 2015 | May–July | Georgia, Texas, and Wisconsin | 90 | Cilantro from Mexico |
| 2016 | June–July | Texas | 6¶¶ | Carrots or green cabbage (suspected) |
| 2017 | May | Florida | 6 | Berries (suspected) |
| 2017 | May–July | Texas | 38*** | Scallions (i.e., green onions) |
| 2017 | June | Michigan | 29 | |
| 2017 | June | Tennessee | 4††† | |
| 2017 | June | Connecticut | 3 | |
| 2017 | July | Florida | 3‡‡‡ |
* The entries in the first three columns refer to the known or likely year(s), month(s), and jurisdiction(s) in which the exposure(s) to Cyclospora occurred.
† The case counts include laboratory-confirmed and probable cases of cyclosporiasis. By definition, each outbreak included at least two linked cases, at least one of which was laboratory confirmed.
‡ A food vehicle is specified only if a single ingredient or commodity was identified in an outbreak investigation.
¶ Cases that occurred in Canadian travelers to the United States were not included.
** An additional 10 probable cases were associated with this outbreak but were not counted in the table: nine of these cases were in residents of states in which cyclosporiasis was not a reportable condition, and the other case was in a patient whose state of residence was unknown.
†† For additional details, see summary information about the outbreak investigations in 2013. For the purposes of this table, the exposure month(s) and case counts are limited to those explicitly linked in the investigations to the food item specified in the last column.
‡‡ For additional perspective, see summary information about outbreak investigations in 2014. For the purposes of this table, the exposure months and the case count for the outbreak in Texas are limited to those explicitly linked in the investigations to the food item specified in the last column.
¶¶ An additional nine suspected cases were identified in persons associated with this outbreak but were not counted in the table because of reporting issues (e.g., insufficient case data).
*** An additional three probable cases were identified in persons associated with this outbreak but were not counted in the table because of reporting issues (e.g., insufficient case data).
††† An additional two probable cases were identified in persons associated with this outbreak but were not counted in the table because of reporting issues (e.g., insufficient case data).
‡‡‡ One additional probable case was identified in a person associated with this outbreak but was not counted in the table because of a reporting issue.
⁂ More information to help distinguish among types of peas can be found here









