The federal Centers for Disease Control and Prevention (CDC) in Atlanta has tracked state outbreaks of Hepatitis A for the last three years, and it is not getting any prettier.
CDC Tuesday reported that 29 states have publicly reported 24,280 hepatitis A illnesses since 2016 with 14,525 or 60 percent requiring hospitalization. And the death toll stands at 236.
Like their state and local colleagues, CDC recommends getting the hepatitis A vaccine as the best way to prevent getting the viral liver disease.
And CDC has identified the activities that can put someone in a category with the highest risks for acquiring HAV infection or developing a serious complication from the HAV infection.
In areas experiencing a hepatitis A outbreak, CDC recommends public health officials offer the vaccine to prevent and control the outbreak. The vaccine is effective for up to two weeks after exposure.
Here’s who is most at risk:
-
- People who use drugs (injection or non-injection)
- People experiencing unstable housing or homelessness
- Men who have sex with men (MSM)
- People who are currently or were recently incarcerated
- People with chronic liver disease, including cirrhosis, hepatitis B, or hepatitis C
Patrons of restaurants that happen to employ one or more infected food service workers are also often caught up in hepatitis A outbreaks. Usually, the local health department or the restaurant offers vaccines to customers who were put at risk of exposure.
As for the vaccine, CDC notes that:
- One dose of single-antigen hepatitis A vaccine has been shown to control outbreaks of hepatitis A and provides up to 95 percent seroprotection in healthy individuals for up to 11 years.
- Pre-vaccination serologic testing is not required to administer hepatitis A vaccine. Vaccinations should not be postponed if vaccination history cannot be obtained or records are unavailable.
In response to all hepatitis outbreaks, CDC says it provides ongoing epidemiology and laboratory support as well as support on vaccine supply and vaccine policy development.
When requested, CDC sends “disease detectives” to affected areas to evaluate and assist in an outbreak response. CDC alerts other public health jurisdictions of any increases in disease. All jurisdictions are encouraged to be watchful for increases in hepatitis A cases. CDC also works with state and local health officials to ensure hepatitis A vaccine is targeted to the correct at-risk populations and that supply is adequate.
State-Reported Hepatitis A Outbreak Cases as of August 16, 2019
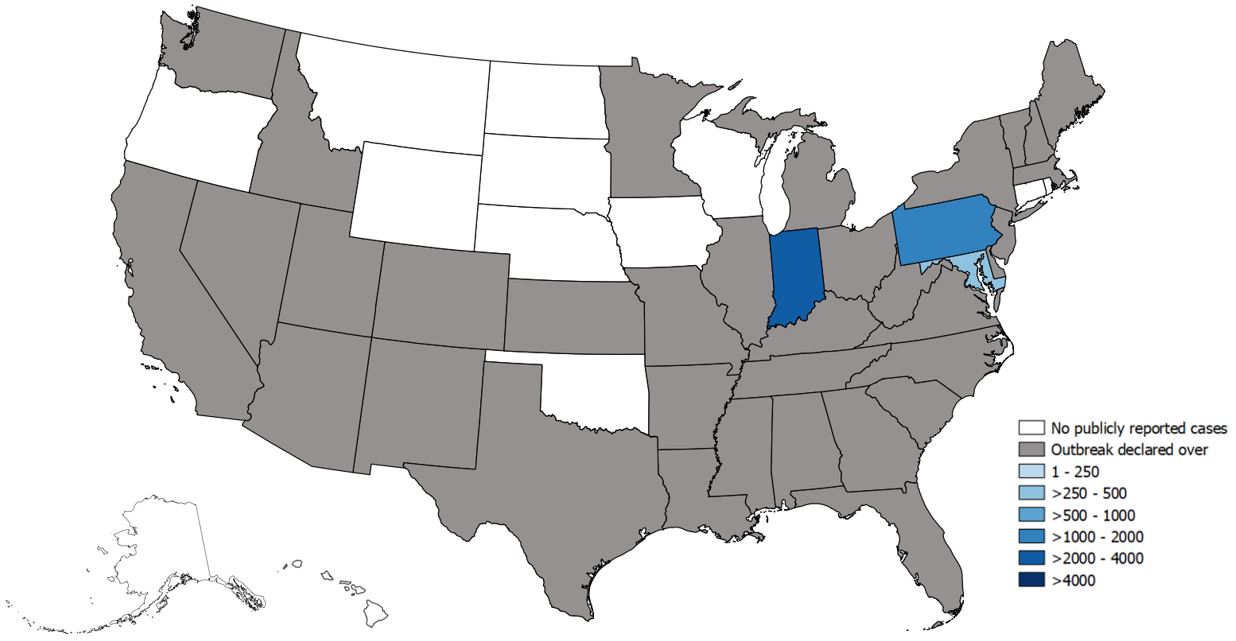
State-Reported Hepatitis A Cases and Clinical Outcomes
| State | Case Total |
Hospitalizations n (%) |
Deaths |
Outbreak Start Date |
Data Current Through |
| Total | 24280 | 14525 (60%) | 236 | ||
| States with an ongoing outbreak | |||||
| Alabama | 132 | 74 (56%) | NR | 9/1/2018 | 8/14/2019 |
| Arizona | 537 | 424 (79%) | 6 | 11/1/2018 | 8/15/2019 |
| Arkansas | 399 | 200 (50%) | 3 | 2/7/2018 | 8/16/2019 |
| Colorado | 123 | 89 (72%) | 0 | 10/1/2018 | 8/14/2019 |
| Florida | 2586 | 1859 (72%) | 31 | 1/1/2018 | 7/31/2019 |
| Georgia | 576 | 391 (68%) | 3 | 6/1/2018 | 8/10/2019 |
| Idaho | 43 | 23 (53%) | 0 | 1/1/2019 | 8/15/2019 |
| Illinois | 150 | 98 (65%) | 1 | 9/1/2018 | 8/14/2019 |
| Indiana | 1995 | 1097 (55%) | 4 | 11/1/2017 | 8/16/2019 |
| Kentucky | 4837 | 2340 (48%) | 60 | 8/1/2017 | 8/3/2019 |
| Louisiana | 468 | 271 (58%) | 1 | 1/1/2018 | 8/16/2019 |
| Massachusetts | 494 | 392 (79%) | 7 | 4/1/2018 | 8/9/2019 |
| Michigan | 918 | 737 (80%) | 28 | 8/1/2016 | 8/14/2019 |
| Minnesota | 24 | 14 (58%) | 0 | 12/16/2018 | 8/9/2019 |
| Mississippi | 25 | 15 (60%) | 0 | 4/1/2019 | 8/12/2019 |
| Missouri | 406 | 226 (56%) | 2 | 9/1/2017 | 8/13/2019 |
| New Hampshire | 174 | 101 (58%) | 1 | 11/1/2018 | 8/13/2019 |
| New Jersey | 323 | 222 (69%) | 3 | 12/1/2018 | 8/10/2019 |
| New Mexico | 136 | 107 (79%) | 2 | 11/8/2018 | 8/15/2019 |
| North Carolina | 87 | 60 (69%) | 1 | 1/1/2018 | 7/15/2019 |
| Ohio | 3244 | 1979 (61%) | 15 | 1/1/2018 | 8/12/2019 |
| Pennsylvania | 376 | 291 (77%) | 7 | 1/1/2018 | 8/10/2019 |
| South Carolina | 291 | 199 (68%) | 1 | 11/1/2018 | 8/12/2019 |
| Tennessee | 2257 | 1350 (60%) | 13 | 12/1/2017 | 8/16/2019 |
| Virginia | 134 | 84 (63%) | 0 | 1/1/2019 | 8/15/2019 |
| Washington | 16 | 11 (69%) | 0 | 4/1/2019 | 8/16/2019 |
| West Virginia | 2540 | 1255 (49%) | 23 | 3/19/2018 | 8/16/2019 |
| States with a declared end to their outbreak | |||||
| California | 708 | 464 (66%) | 21 | 11/1/2016 | 4/11/2018 |
| Utah | 281 | 152 (54%) | 3 | 5/8/2017 | 2/12/2019 |
NR: not publicly reported
- “Outbreak-associated” status is currently determined at the state level in accordance with each state’s respective outbreak case definition.
- Outbreak-related hepatitis A deaths are defined at the state level in accordance with each state’s respective hepatitis A-related death definition. Some states are reviewing death certificates on a regular basis to actively find hepatitis A-related deaths, while other states are utilizing passive surveillance.
- Outbreak start date is defined at the state level and may represent the earliest onset date of an outbreak case (AR, AZ, UT), the left censor date for which cases are considered part of the outbreak based on the state outbreak case definition (AL, CA, CO, FL, GA, ID, IL, IN, KY, LA, MA, MI, MN, MO, MS, NC, NH, NJ, OH, PA, SC, TN, VA, WA), or when a state declared a hepatitis A outbreak (NM, WV).
(To sign up for a free subscription to Food Safety News, click here.)









