The number of reported cases of domestically acquired cyclosporiasis illnesses has increased by 254 cases since the last update on July 14, 2021. Cases continue to be reported to the Centers for Disease Control and Prevention.
As of July 27, there have been 462 laboratory-confirmed cases of cyclosporiasis in people who had no history of international travel during the 14-day period before illness onset. The ill people have been reported to CDC by 29 jurisdictions, including 28 states and New York City.
Illness onset dates range from May 1 to July 16. However, there are likely more infected patients, officials say, because of the lag time between a person becomes ill and when confirmed test results reach federal officials.
At least 41 people have been hospitalized; no deaths have been reported.
Cyclosporiasis illnesses develop from infections by the Cyclospora parasite, a microscopic organism. Illnesses are reported year-round in the United States. However, during the spring and summer months there is often an increase in cyclosporiasis acquired in the United States. The exact timing and duration of these seasonal increases in domestically acquired cyclosporiasis can vary, but reports tend to increase starting in May.
In previous years the reported number of cases peaked between June and July, although activity can last as late as September. The overall health impact, such as the number of infections or hospitalizations), and the number of identified clusters of cases i.e., cases that can be linked to a common exposure, also vary from season to season.
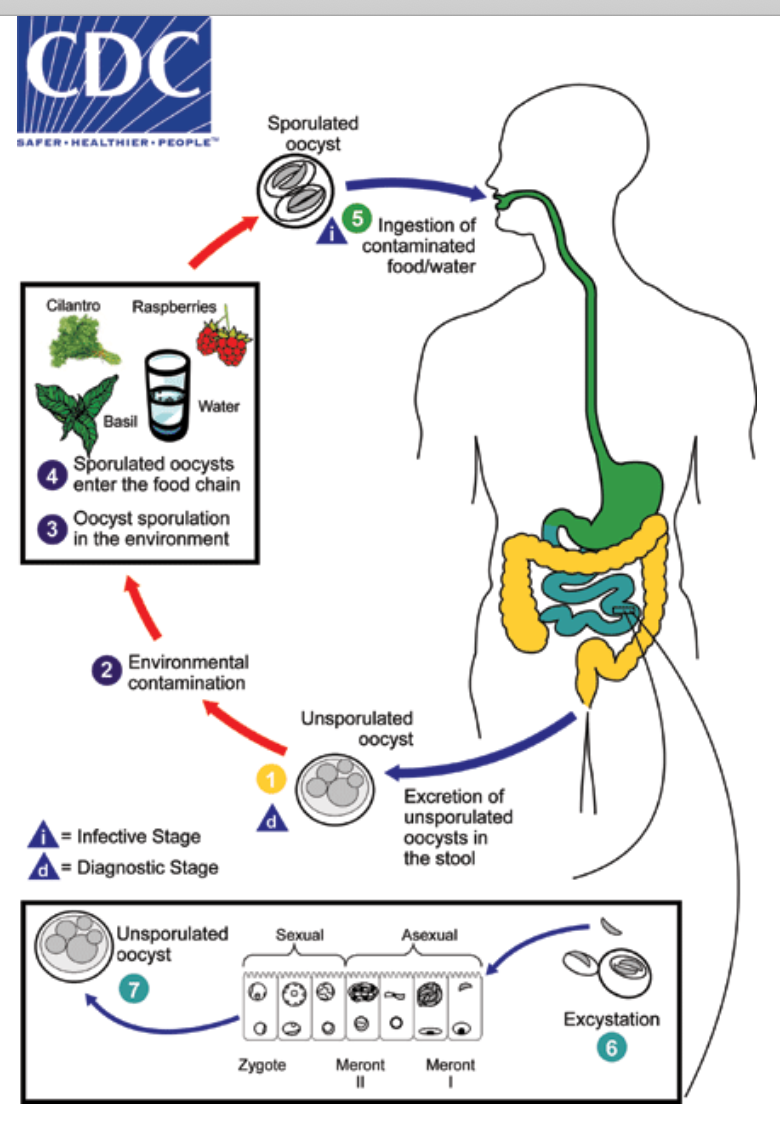
Previous U.S. outbreaks of cyclosporiasis have been linked to various types of fresh produce, including basil, cilantro, mesclun lettuce, raspberries, and snow peas.
The CDC, along with state and federal health and regulatory officials, monitor cases of cyclosporiasis in the United States in the spring and summer months to detect outbreaks linked to a common food source.
However, many cases of cyclosporiasis cannot be directly linked to an outbreak, in part because of the lack of validated laboratory “fingerprinting” methods needed to link cases of Cyclospora infection.
Officials use questionnaires to interview sick people to determine what they ate in the 14-day period before illness onset. If a commonality is found, CDC and partners work to determine if a contaminated food product is still available in stores or in peoples’ homes.
Cyclospora cayetanensis is a unicellular, microscopic parasite that can cause food- or water-related gastrointestinal illness. Cyclospora cannot be transmitted directly from one person to another through infected fecal matter; the parasite must complete part of its lifecycle outside of a host. Most cases of cyclosporiasis occur in underdeveloped tropical and subtropical regions of the world where the parasite is endemic.
In the United States, Cyclospora causes about 11,000 illnesses and 11 hospitalizations, but infestations of this parasite do not typically result in death. Due to the self-limiting nature of the pathogen, which causes some people to not seek medical care, difficulty in diagnosing it specifically, and other factors, the Centers for Disease Control and Prevention estimates that there could be very broad ranges of infection, from 140 to 38,000 annual cases.
In North America, outbreaks of cyclosporiasis in humans have been reported mostly from contaminated fresh food products, such as soft fruits like raspberries, blackberries, and strawberries, leafy vegetables including lettuce and mixed salad, and herbs such as basil and cilantro.
Since Cyclospora infections tend to respond to the appropriate treatment, complications are more likely to occur in individuals who are not treated or not treated promptly. These can include disorders of malabsorption, reactive arthritis, inflammation of the gallbladder, and, possibly, Guillain-Barré Syndrome.
(To sign up for a free subscription to Food Safety News, click here.)









