Over 200 died, many were the young and the unborn who will never turn 4.
In March of this year it will be 4 years since I boarded a flight from Seattle to Johannesburg (20 plus hour flight) to speak at a food safety conference just days after the South African health authorities announced that a Listeria outbreak had been linked to a product named polony manufactured by the largest food manufacturer in Africa.
I recall how similar it felt to the early days of the Jack-in-the-Box E. coli outbreak of 1993– how everyone seemed honestly shocked that such a tragedy could happen.
I have spent the last 4 years working (being 10 hours behind has required far too many late nights and early morning calls) with a cadre of amazing lawyers and more amazing staff moving forward in the first foodborne illness class action in Africa. We have much to do to find justice to the more than 1,000 sickened and their families. I am saddened by the pace of the litigation, but determined to take care of our class members – we have to work harder.
Sadly, what I warned about in 2013 came to pass.
Section 61 of the Consumer Protection Act, 2008 (“CPA”) provides that producers, importers, distributors and/or retailers of goods (collectively the “supplier(s)”) may be held liable for any harm caused as a result of the supply of unsafe goods, product failure, a defect or hazard in the product, inadequate instructions for the use of goods or warnings related to any possible hazard that might be associated with the product, whether or not there was “fault” on the part of the supplier.
BACKGROUND
In 2017 and 2018, the world’s largest and deadliest outbreak of listeriosis occurred in multiple provinces of South Africa, as seen in Figure 1. The outbreak was caused by contaminated polony, a ready-to-eat, processed meat product. Ready-to-eat, processed meats are a well-known vehicle for listeriosis outbreaks (Thomas et al., 2020). The Minister of Health declared that there was an outbreak of listeriosis on December 5, 2017, that was linked to polony emanating from Tiger Brands’ Enterprise Foods production facility in Polokwane on March 4, 2018.

Figure 1. Incidence of Laboratory-Confirmed Listeriosis Cases during the Outbreak Period, According to South African Districts (Thomas et al., 2020).
Cases were reported from across the country, with most cases reported from Gauteng Province (58%). Women accounted for 55% of total cases. The ages of cases ranged from birth to 93 years. Neonates (aged £ 28 days) were the most affected age group, accounting for 43% of cases. This was followed by adults of 15 to 49 years of age, accounting for 32% of cases. The disease outcome was known for 806/1,060 (76%) of cases; 27% (216/806) had the known outcome “died” (Smith et al., 2019).
Listeriosis is a serious foodborne infection with a case-fatality rate (“death rate”) of 20-30% (Thomas et al., 2020). People primarily affected by listeriosis have impaired cell-mediated immunity. This includes those who are pregnant, elderly, or immunocompromised from conditions such as HIV, chronic disease, or immunosuppressive therapy (Thomas et al., 2020). The specific outbreak strain associated with the outbreak was Listeria monocytogenes sequence type 6 (LmST6). There are two ways that listeriosis can manifest: febrile gastroenteritis and invasive listeriosis (Coulombier). Invasive listeriosis is characterized by bacteremia, meningitis, pneumonia, endocarditis, and sepsis (Smith et al., 2019).
A total of 1,060 cases were reported during the outbreak period of January 11, 2017, to July 17, 2018 (Figure 2). The outbreak period was defined as a duration of time during which case numbers exceeded and remained above a weekly threshold of five cases per epidemiological week (Thomas et al., 2020). At the peak of the outbreak (mid-November 2017), 41 listeriosis cases were reported in a single week. Prior to this outbreak, listeriosis was not a reportable disease in South Africa; therefore, information is not available on the prevalence, epidemiology, and description of clusters/outbreaks on listeriosis. Due to the lack of surveillance data, the baseline number of listeriosis cases was estimated from counts of listeriosis cases in 2016.
It is known that in 2015 and 2016, clusters of listeriosis occurred in South Africa. The 2015 listeriosis cluster involved 7 cases total, and the predominant strain was Lm ST6. However, researchers found that the 2015 cluster did not constitute an outbreak (Shuping et al., 2015). For the 2016 cluster, retrospective analysis of Lm cases from the years 2012-2016 was used to calculate the expected case numbers for years 2013, 2014, 2015, and 2016 in the Gauteng province (Mathebula et al., 2016). Because there were only 3 cases in the 2016 outbreak, researchers needed to estimate the baseline number of cases. When determining if a cluster of diseases is classified as an outbreak or epidemic, it is essential to know what the baseline number of illnesses is in the population of interest. An epidemic refers to an increase in the number of cases of a disease, above what is normally expected in that population in that area, and an outbreak is defined the same but is often used for a more limited geographic area (Center for Disease Control and Prevention [CDC], 2012).
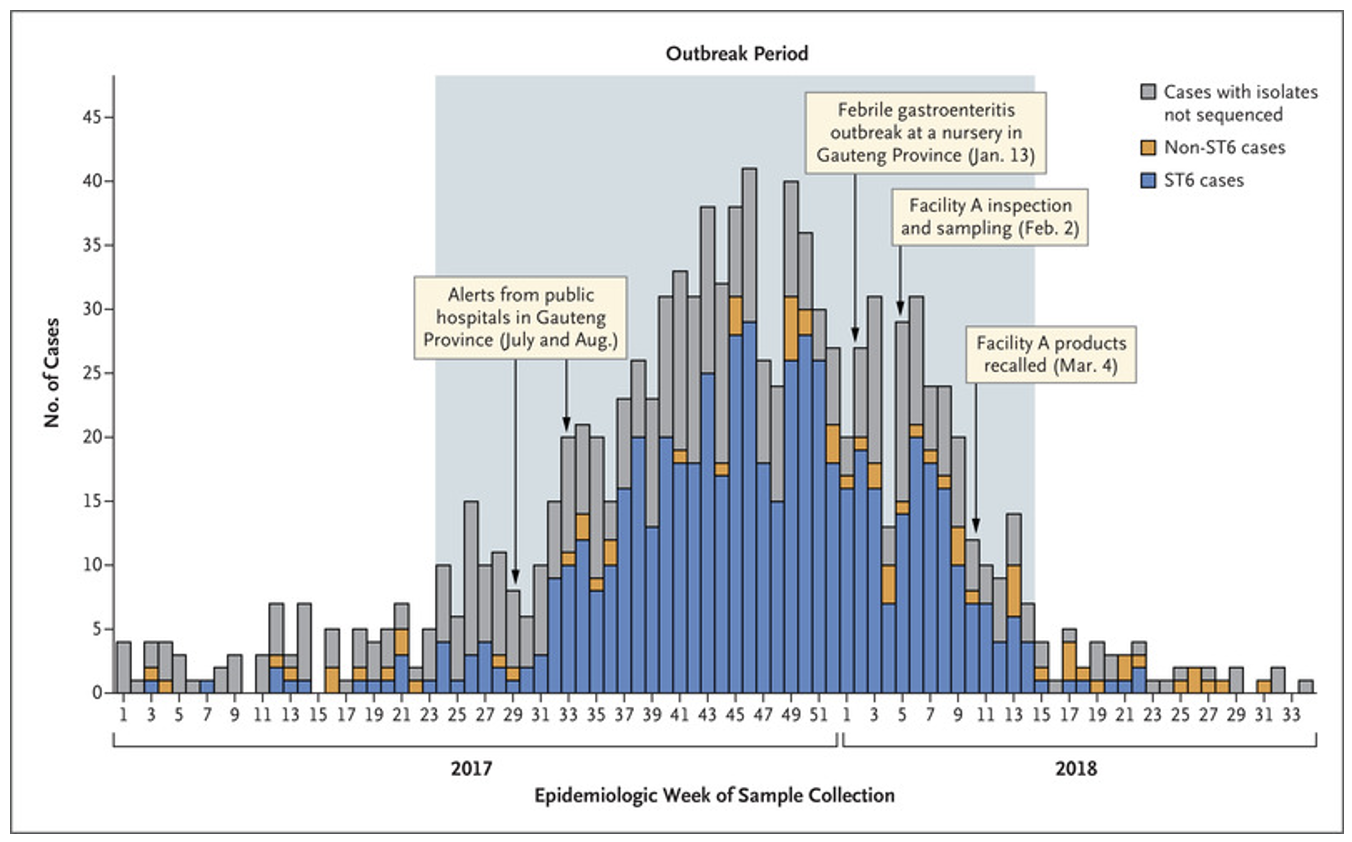
Figure 2. Distribution of Laboratory-Confirmed Cases of Listeriosis, According to Outbreak Week and Major Events (January 1, 2017 to August 21, 2018) (Thomas et al., 2020).
CASE IDENTIFICATION AND MICROBIOLOGICAL INVESTIGATION
Case definitions are used in outbreak investigations to help identify cases who are associated with the outbreak. A case definition includes criteria such as the subject population, implicated location, time, clinical features, and/or laboratory test results if available (CDC, 2012).
The initial case definition for this outbreak included all cases of listeriosis that occurred in South Africa from 2017 to 2018. The initial case definition was appropriate due to the lack of whole-genome sequencing (WGS) data at the beginning of the outbreak. Multilocus sequencing typing (MLST) was used after to analyze the WGS results. Researchers discovered that 93% of the clinical isolates collected from cases in the outbreak period were Listeria monocytogenessequence type 6 (Lm ST6) (Thomas et al., 2020; Gerner-Smidt). The case definition later included sequence typing information to increase the likelihood of identifying a common source (Besser). This finding also showed that the outbreak was centered around the ST6 strain, meaning that any person infected with the ST6 strain, in South Africa, could have been considered a victim of this outbreak during the outbreak period, before the outbreak period (when the environmental samples tested positive for ST6), and after the outbreak period (when contaminated products could have still been present in homes) (Coulombier).

Figure 3. NCBI WGS Tree.
Although microbiological evidence is useful, a case definition without subtyping information can still be adequate in solving an outbreak (Besser). Multiple factors can be taken into consideration to determine if a case is associated with an outbreak regardless of if they were laboratory confirmed or not. As stated above, 93% of clinical isolates were ST6; however, not all isolates could be sequenced, due to the lack of laboratory resources and personnel available (Besser). Based on the high percentage of ST6 clinical isolates, we can assume that a similar number of non-sequenced isolates would have been classified as ST6 if sequencing could have been done (Coulombier). Another reason that we can assume that there is no difference between the distribution of sequence types among the non-sequenced samples and the distribution of sequence types observed in the sequenced samples is because the process of selecting case isolates to be sequenced was not biased. In the absence of other information, a listeriosis patient diagnosed during the outbreak period had a > 90% probability of being related to the outbreak even without confirmed laboratory results (Gerner-Smidt).
EPIDEMIOLOGIC INVESTIGATION
After detection of the outbreak, the Centre for Enteric Diseases, a part of the National Institute for Communicable Diseases, conducted a nested, case-control study that provided evidence that cases with Lm ST6 infections were more likely to have eaten polony than those with non-ST6 infections (Thomas et. al, 2020). In outbreak investigations, case-control analysis is performed to estimate the odds ratio for the association between specific food items and the outbreak-associated illness. For this nested case-control study, case patients were those with Lm ST6 infections, and control patients were people with non-ST6 listeriosis during the outbreak period. Results from this study show that the odds ratio was 8.55 with a 95% confidence interval of 1.66 – 43.35. An odds ratio is a measure of association between the odds of getting ill having consumed a specific food item versus the odds of being ill having not consumed the specific food item (Coulombier). An odds ratio of 8.55 signifies that the odds of having eaten polony in ST6 cases is 8.55 times greater than the odds of having eaten polony in non-ST6 cases. From the calculated confidence interval, we know that this result is significant because the confidence interval does not include the null value of 1, and that 95% of the time we can expect the true odds ratio to fall within this interval.
Prior to the study, food history interviews were conducted to generate a hypothesis about which foods could have been the source of the outbreak (Coulombier). The food histories were conducted with the use of a standardized questionnaire that investigated foods consumed four weeks prior to onset of symptoms. Open and close-ended questions were utilized in the interview to prevent bias. The food history interviews were completed by November 1, 2017. The epidemiology methods utilized in this investigation mirrored those used in high-level investigations throughout the world and were fully appropriate for the outbreak circumstances (Besser).
ENVIRONMENTAL INVESTIGATION
On January 13, 2018, febrile gastroenteritis developed in 10 children from a nursery in Gauteng Province. Several stool samples were collected from the children, and one yielded L. monocytogenes ST6. Sandwiches prepared and eaten at the nursery were the only common food exposure, and polony was the common ingredient. Polony was recovered from the nursery refrigerator, and L. monocytogenes ST6 was identified in the polony produced at Tiger Brands Enterprise Facility in Polokwane (Thomas et al., 2020).
On February 2, 2018, an environmental investigation took place at the Tiger Brands Enterprise Facility in Polokwane following the discovery at the nursery (Gerner-Smidt). Of 317 environmental samples taken from the Polokwane facility, 47 tested positive for Listeria monocytogenes, and of the 47 that tested positive, 34 were subtyped as the outbreak ST6 strain. Additionally, two of 13 samples of unopened polony loaves collected at the facility tested positive for Listeria monocytogenes, and both were subtyped as the outbreak ST6 strain. Extensive environmental investigation took place in an additional 148 ready-to-eat food manufacturers, but the outbreak strain was not identified at any of the other manufacturer locations. The outbreak strain of Lm ST6 was only found at the Tiger Brands Enterprise Facility in Polokwane. This finding suggests that the Enterprise Facility was more likely than not to be the source of the outbreak (Gerner-Smidt).
DISCUSSION
By incorporating findings from the epidemiology, microbiology, and traceback data, experts were able to provide strong evidence that the source of the outbreak was polony produced from Tiger Brands Enterprise Foods Polokwane production facility. The Minister of Health declared the source of the outbreak on March 4, 2018, which led to the recall of the contaminated polony. The recall of the contaminated polony resulted in a substantial decrease in cases of listeriosis in South Africa. By mid-April 2018 (6 weeks after recall), fewer than 5 cases were reported weekly. The outbreak was considered over on September 3, 2018 (Thomas et al., 2020).

REAL STORIES
The victims of the 2017 listeriosis tragedy and the surviving families of those who died are taking on Tiger Brands to win some form of justice and force some form of accountability. A Maverick Citizen team travelled to all four corners of South Africa to tell the stories of the claimants who are fighting back.
Carla Verlaat, 23
Carla Verlaat lost her first baby in 2017. She went into premature labor at 22 weeks. Her son Shem only lived for 24 hours before he died. The doctors told Carla her baby had a clot in his brain, and he was later diagnosed with listeriosis.

Carla Verlaat at home in Manenburg, Cape Town.At 22 weeks pregnant, Carla lost her baby, Shem. Shem was diagnosed as having listeriosis. (Photo: Thom Pierce)
Carla cries as she speaks about the pain of her milk running out of her breasts intended for a baby who had died. She has a single picture of Shem on her phone. He is lying in an incubator, with many pipes attached to his fragile body, his face a dark grey. Since Shem passed away, Carla has battled with her grief. Despite having gone to therapy, she still struggles to manage her mood swings. Sometimes she stabs her bedroom door with a knife, in an attempt to find some kind of release. She blames herself for Shem’s death and is too afraid to have another baby.
Annelize le Roux, 42
Annelize le Roux lost her “miracle baby”. The year before giving birth to her miracle, she terminated another pregnancy when told the unborn baby had Down’s syndrome. She was told that she would never have another child. Being subsequently pregnant with her son Andreas was an unexpected but happy surprise. The family was devastated when Andreas died.

Annelize and Martin Le Roux with their dog Max and their pet lion Caesar on their farm in Winburg, Free State. Annelize suffered a miscarriage at 23 weeks, their baby boy was later diagnosed with listeriosis. (Photo: Thom Pierce)
Before Andreas died, Annelize’s whole family fell ill. “It was just like strong flu symptoms,” she said. Her husband Martin did not think much of his illness. Annelize, who is a microbiologist, was determined to find out what happened. So, after Andreas died, they sent his blood for tests to England. The results confirmed that Andreas had contracted listeriosis while in his mother’s womb. When Annelize found out about the outbreak, she isolated and packaged foodstuffs from her fridge. When the health inspectors came to her home, she had prepared all the samples for them. This played a crucial role in assisting the health department in confirming the source of the contaminated foodstuffs.
Amelia Govender, 28, and Kyle Victor, 26
Amelia and Kyle were incredibly excited for the arrival of their baby girl, Summer Reign. They both describe the birth of their little girl as the best day of their lives. Kyle, who had initially hoped for a boy, fell in love with his daughter at first sight. “I saw her, and I just thought, ‘why did I ever want a boy?’”

Kyle Victor and Amelia Govender at their home in Kingsburgh, KwaZulu-Natal. At one day old, their daughter Summer Reign died from listeriosis. For the last two years Amelia has suffered severe health complications brought on by listeriosis. (Photo: Thom Pierce)
Amelia and Kyle had been thoroughly prepared for their baby. Amelia had bought little outfits for Summer Reign; she’d even got her a Louis Vuitton designer baby blanket. She became worried when her baby’s movements started to wane. That was the first sign of trouble. A few days later, Summer died. She and Kyle were devastated. Amelia has tears in her eyes as she talks about how she prayed that her baby would wake up during her funeral, but Summer was gone.
Since then, Amelia has dealt with debilitating health issues. Every morning, she wakes up to a swollen face, and often her lower body breaks out in an itchy rash that leaves welts all over her. She still has not been able to figure out the cause of her symptoms.
Meryl Kothiah, 38
Meryl and her husband were looking forward to having their first child together in 2017. Shabeer immediately started a separate savings account to cater for the baby’s future needs. Seven months into her pregnancy, Meryl started to feel ill. She struggled with fever on and off, until the doctors told her they would have to perform an emergency Caesarean section.

Meryl and Shabeer Kothiah at home in Shallcross, KwaZulu-Natal. At seven months, Meryl had to have an emergency Caesarean section and gave birth to a boy, Saiheer. Saiheer died less than 24 hours later. He was diagnosed with listeriosis. (Photo: Thom Pierce)
Baby Saiheer was born on 28 November 2017 and, as far as Meryl was aware, the baby was healthy. When her husband arrived at the hospital to see her and the baby, he found little Saiheer dead. Saiheer had lived less than a day before he died due to a listeriosis infection contracted while in his mother’s womb. After Meryl was discharged from the hospital, she started to notice that she was getting severe allergic reactions, especially when it was hot. Her skin would start to itch badly, and welts would develop where she scratched. She also described her face swelling up, so much so that she is afraid of leaving the house. “I don’t want people to see me like that,” she said.
Johan Keiser, 65

Johan Keiser at home in Forest Hill, Gauteng. In late 2017, Johan was rushed to hospital where he spent a total of 25 days, 12 of which were in the hospital intensive care unit. He was diagnosed with listeriosis and considers himself lucky to be alive. (Photo: Thom Pierce)
Johan Keiser considers himself “one of the lucky ones”. The 65-year-old pensioner fell ill and was taken to hospital by his wife. He has no recollection of being in the hospital for 25 days, 12 of which he spent in the hospital’s intensive care unit. “I took polony with cheese, lettuce and tomatoes to work every single day, and it almost cost me my life,” he said. While Johan has made a full recovery, he notes that he has a weakness in his legs, making it difficult for him to get up when sitting. He has high praise for the doctors who attended to him. “I am so grateful that they pulled me through because, according to me, I was a dead person for 20 days,” he says.
Anetta Masie, 44

Anetta Masie at home in Xihoko, Limpopo. Anetta spent two weeks in hospital being treated for listeriosis after her one-day old baby died from the infection. (Photo: Thom Pierce)
Anetta Masie held her baby girl only once before she died. The infant contracted listeriosis in her womb and died soon after birth. As the baby was premature and weighed less than a kilogram, the fetus was disposed of as medical waste. She was unable to have a funeral for her child. She was discharged the same day and told to come back at a later stage to have her womb cleaned. Anetta spent at least two weeks in hospital being treated for listeriosis with antibiotic intravenous drips. When she finally returned home to Limpopo, accompanied by her husband Thomas, her two elder children were devastated to find that she did not come home with a baby. “Losing my baby was so painful, especially because I didn’t really know what killed my baby,” said Anetta. Since the death of her baby girl, Anetta does not eat any Enterprise products. She is terrified that she will get ill again.
Christina Ledwaba, 31

Christina Ledwaba at home in Mankweng, Limpopo. Since losing her baby, Mohau, to listeriosis, Christina has managed to give birth to a healthy baby girl. (Photo: Thom Pierce)
“I knew something was wrong the minute I saw that sonar,” she said. Doctors confirmed that the baby had no heartbeat. She then gave birth to Mohau. When the baby was delivered, the nurses merely left the umbilical cord attached. For hours she lay on the bed with her dead baby under her legs. Since then, Christina has had another baby, but when she was eight months pregnant, she experienced diarrhea and started to panic, worried that something was wrong again, but she was able to give birth to a healthy little girl. Despite good evidence that her stillborn baby’s death was linked to listeriosis, Christina still consumes Enterprise products, but she makes sure that the food is heated first.
Stephen Thokwane, 43
Stephen Thokwane is a shadow of his former self. The once fit and healthy man fell ill in December 2017. What started off as a headache and flu-like symptoms turned into a nightmare for his family.

Stephen Thokwane at his home in Steelpoort, Limpopo where he lives with his wife and four children. Once fit and healthy, Stephen contracted listeriosis and is now a shadow of his former self. (Photo: Thom Pierce)
Dumbfounded by his sudden illness, which he self-diagnosed as a stroke, the family first sought spiritual help. The family said that the prophet told the family that they needed to pray for Stephen. Stephen deteriorated and he was admitted to hospital, where he lost his eyesight, suffering severe delirium and temporary paralysis. The man, who used to jog 15 kilometers at a time, found himself having to learn how to walk again. And while he is back on his feet, his health is still not what it was. He is fatigued, and he has lost strength. Due to this, he is no longer able to continue his work as a boilermaker, something he did part-time besides his formal employment, in order to support his family. Thokwane is now working towards paying off a loan he took out to build a house for his wife and four kids. “After he got so sick, he was worried that he may die without leaving us with a roof over our heads, so he took out a loan to build this house,” his wife Maggi said.
Monthla Ngobeni, 37
Monthla Ngobeni is the first named claimant in the court papers. Her daughter Thetho, who is almost two, has undergone four operations since she was born. After contracting listeriosis in her mother’s womb, Thetho developed a condition called Hydrocephalus, a build-up of fluid in the brain. A shunt that drains the fluid has been inserted into Thetho’s head in order to manage her condition and, ultimately, save her life. She will always have a shunt and it will have to be replaced periodically as she grows.

Monthla Ngobeni with her daughter, Thetho, at home in Polokwane, Limpopo. Montlha is the first named claimant in the listeriosis class action. Thetho was born with severe health complications due to contracting listeriosis in the womb. (Photo: Thom Pierce)
The shunt has been blocked twice so far, forcing the little girl to undergo surgery to remove and replace it. Doctors have told Monthla that Thetho’s development milestones will be significantly delayed. At two, Thetho cannot speak yet. There is no certainty of what the future holds for her. Monthla has fallen into debt trying to manage both her and Thetho’s medical bills. She currently owes a hospital R26,000 for a hip replacement that she needed due to her own listeriosis infection.
Ephraim Chinula, 64

Ephraim Chinula, Riley’s grandfather, at home in Eldorado Park, Soweto. After his grandson fell ill along with nine other children from their creche, Ephraim rallied the community, and the result has been the listeriosis class action. (Photo: Thom Pierce)
Ephraim Chinula is Riley Chinula’s grandfather. Riley Chinula contracted Listeriosis alongside nine other children after eating contaminated meat at their creche in Soweto. The stools from the sick children were investigated and led to the first confirmation of the listeriosis outbreak.
Riley, who was three years old at the time, was the youngest of the kids at the creche. They all had high fevers, stomach cramps, vomiting and diarrhea. The entire group was taken to Chris Hani Baragwanath hospital, where doctors were ready to receive them.
“I got the impression that the doctors knew what they were dealing with, as they had been briefed by the local clinic, so they already suspected listeriosis.” Laboratory tests were run on the kids, and it was confirmed that the children had indeed contracted listeriosis. When the news broke, the community came together and committed themselves to seeking justice for what they viewed as negligence on the part of Tiger Brands.
Tebogo Ntjana, 31

Teddy and Tebogo Ntjana at home in Midrand, Johannesburg. They lost their second daughter to listeriosis, Tebogo and Teddy are still searching for closure. (Photo: Thom Pierce)
Tebogo became very ill in October 2017 and was taken to hospital where she later suffered a miscarriage, four months into her pregnancy. The doctors took blood samples and told her that she had contracted listeriosis. Not knowing anything about the illness, Tebogo and her husband, Teddy, searched online for it and were alarmed to discover the severity of the condition. “We googled listeria … yoh, we got scared.”
Thinking that it was a singular case, they presumed that they had done something to cause the illness. One month later, the couple heard the then minister of health, Dr Aaron Motsoaledi, announcing the listeriosis outbreak on the radio. The news came as a relief to the couple who would often buy polony and viennas from a Tiger Brands factory shop in Germiston. They have been blaming themselves for the miscarriage since it happened. “You blame yourself as if you killed your baby,” Tebogo said.
This piece of both journalism and photojournalism by Nomatter Ndebele and Thom Pierce of the Maverick Citizen.
References
Besser, J. (2020). Expert Opinion Regarding a Listeria Outbreak in South Africa Involving Tiger Brands Limited.
Coulombier, D. (2020). Expert Opinion Regarding a Listeria Outbreak in South Africa Involving Tiger Brands Limited.
Food Focus. (2017). An overview of the Listeria outbreak in South Africa (fact sheet).
Gerner-Smidt, P. (2020). Expert Opinion on Subtyping Aspects of the Listeria Outbreak in South Africa Involving Tiger Brands Limited.
NICD. (2016). Investigation of Listeria monocytogenes cases at Charlotte Maxeke Johannesburg Academic Hospital in Johannesburg, December 2016.
NICD. (2017). Investigation of Listeria monocytogenes cases identified at Tshwane academic laboratory, 1 March-30 August 2017.
NICD. (2018). The Listeria outbreak: Meeting with RSA extended stakeholders and WHO Listeriosis team (PowerPoint presentation).
Shuping, L., et al. (2015). Investigating a cluster of Listeria monocytogenes cases in the Western Cape province of South Africa, September 2015.
Smith, A. M., et al. (2016). Genome Sequences for a Cluster of Human Isolates of Listeria monocytogenes Identified in South Africa in 2015. Genome Announc. 4(2): e00200-16. doi:10.1128/genomeA.00200-16.
Smith, A. M., et al. (2019). Outbreak of Listeria monocytogenes in South Africa, 2017-2018: Laboratory Activities and Experiences Associated with Whole-Genome Sequencing Analysis of Isolates. Foodborne Pathog. Dis. 16(7): 524-530. doi:10.1089/fpd.2018.2586.
Thomas, J., et al. (2020). Outbreak of Listeriosis in South Africa Associated with Processed Meat. N. Engl. J. Med. 382: 632-643. doi:10.1056/NEJMoa1907462.











